How can I stop ringworms on my thighs?
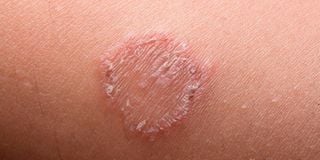
Ringworms are a result of fungal infections, in this case called Tinea Cruris because it is between the thighs.
What you need to know:
- Recurring fungal infections could be due to misdiagnosis, not completing treatment, or a poor immune system
- It could also be due to a genetic condition where the skin does not recognise the fungus as foreign matter
- Many times, the fungi that cause infection usually live naturally on or in our bodies
Dr Flo,
Can you recommend an effective drug to clear ringworms between the thighs? I have tried clotrimazole and terbinafine but the ringworms keep recurring. It is really depressing. Can you recommend a shampoo? What could be the cause?
L M
Dear L M,
Ringworms are a result of fungal infections, in this case called Tinea Cruris because it is between the thighs. The infection is transmitted though physical contact or shared towels or under garments. You can also get it if you remain in sweaty clothes for long. It causes a rash that is itchy or has a burning sensation.
Recurring fungal infections could be due to misdiagnosis, not completing treatment, or a poor immune system. It could also be due to a genetic condition where the skin does not recognise the fungus as foreign matter and, therefore, the body does not try to get rid of it.
Many times, the fungi that cause infection usually live naturally on or in our bodies and only cause a problem when they multiply too much. This also means it is easy to get a fungal infection from another person, since they are also carrying fungi, and also from clothing, towels, lanyards, floors among others. Fungi like warm and wet environments, which is why it is easy to get fungal infections between the thighs, toes, or in the groin.
Fungi also shed spores, which are like tiny seeds that collect in our clothes or shoes, waiting for the right conditions to grow again. This means that if there are spores present, you can have proper treatment and then the infection comes back when the spores start growing.
This condition can be managed, though it may not be possible to get rid of it permanently. You need to visit a dermatologist to get a proper diagnosis. It would also be beneficial to check for any conditions that could lower your immunity like diabetes and HIV. When you are put on medication, take it for the prescribed duration, even if the skin rash has disappeared. You can also take tablets or use a cream or anti-fungal shampoo (such as ketoconazole or clotrimazole) occasionally after treatment to prevent regrowth. You can also apply antifungal powder to the area daily. Keep the area clean and dry, wear loose cotton underwear and pants, and change clothes daily. Clothes should be washed and sun dried in an airy place, and if possible, ironed inside-out. If you have a fungal infection elsewhere on the body such as between the toes, make sure it is also treated. Also, clean your shoes regularly, get rid of old shoes, and wear leather shoes. Any family members or other contacts that have the skin infection should also be treated. Also, avoid sharing clothes, shoes, towels among other personal items.
Dr Flo,
I am allergic to the penicillin and cephalosporin group of antibiotics. Is it safe for people like me to get the Covid-19 AstraZeneca vaccine? Could there be a serious problem?
Wanjiku
Dear Wanjiku,
You can receive the AstraZeneca vaccine since it does not have penicillin or cephalosporin. It has also been found to be safe for people with allergies to multiple classes of drugs. The only concern is if you have a history of allergic reaction to any of the excipients, which include: L-histidine, L-histidine hydrochloride monohydrate, magnesium chloride hexahydrate, polysorbate 80 (E433), ethanol, sucrose, sodium chloride, disodium edetate dihydrate and water for injection.

You can receive the AstraZeneca vaccine since it does not have penicillin or cephalosporin.
Dr Flo,
I have constipation and sometimes pain in my stomach. I also feel weak sometimes. For one month now, my stool has been shiny. I also have chest pains. Two weeks ago, the doctor told me I had iron and Vitamin D deficiency. I am on supplements now but my health is worsening. What can I do? It is like my body is not absorbing food. I am really in pain. Advise me on treatment and the foods I should avoid.
Kevin
Dear Kevin,
Constipation is defined as not passing stool at least once in three days, or often passing dry or hard stool, or often having difficulty pushing out stool. In addition to the constipation, you also have shiny stool, which may be a sign of too much fat in stool. You also have Vitamin D and iron deficiency, weakness, abdominal and chest pain. This combination could be due to a malabsorption disorder where the intestines are unable to absorb certain foods or they are unable to breakdown (digest) these foods properly into what can be absorbed. It could also be due to an inflammatory bowel disease or irritable bowel syndrome.
You should see a gastroenterologist for a comprehensive examination. The treatment will be specific to the diagnosis. Supplements are helpful in correcting the deficiencies, though the iron supplements may worsen the constipation and change the colour of stool.
In the meantime, keep a food and symptom diary to try and identify if there are specific foods that make your symptoms worse.
You can make your stool softer by taking adequate fluids and fibre, which is found in fruits, vegetables and cereals. Also avoid being inactive, for instance, sitting or lying down for long and start exercising. You also need a good toilet routine – go to the toilet at a regular time and place where you are comfortable, use the toilet when you feel the urge to, and you can use something to raise your legs, so that your knees are above your hips when you are sitting on the toilet seat.
Vitamin D is made by the body when sunlight triggers its formation from cholesterol in the skin. It is also found in small amounts in some foods like oily fish, liver, egg yolk, cheese, mushrooms, fish liver oil and foods fortified with Vitamin D. To manage the Vitamin D deficiency, get adequate sunshine exposure (10 to 30 minutes, between 10am and 4pm) at least twice a week.
Foods rich in iron include red meat, chicken and dark green leafy vegetables.
Send your medical questions to [email protected] for free expert advice


