Ministry mulls new Covid-19 booster jabs
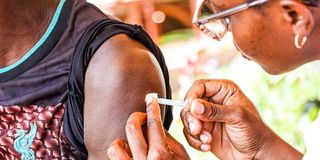
A nurse administers a Covid-19 jab to a youth at Teens Watch Centre in Kwale County.
The Ministry of Health may soon procure Covid-19 vaccine boosters after a new study found that the Sars-Cov-2 virus evolution outpaces vaccine-generated antibodies.
This is after scientists at Oxford University compared two mRNA-bivalent vaccine boosters.
The findings come after a clinical trial where the researchers compared early neutralising antibody responses after boosting with bivalent Sars-Cov-2 mRNA vaccines based on either BA.1 or BA.4/BA.5 Omicron spike protein combined with what they described as a wild-type spike.
“Responses against Sars-Cov-2 variants exhibited the greatest reduction in titres against currently circulating Omicron sub-variants for both bivalent vaccines,” the researchers concluded in their official report.
Speaking to Nation yesterday, Mr Ondari Mogeni, a Kenyan epidemiologist at the International Vaccine Institute (IVI), said the findings underscore the need for Covid-19 booster shots.
“Being preliminary results, there is a need to cautiously interpret them, the evolution of the virus means there is a need for boosters every now and then just like it is done for influenza. Because of many circulating influenza sub-types, vaccines are in each season tailored to the predominant sub-types that are circulating,” he said.
“We first need to examine immunity to determine after how long boosting should be done,” Mr Mogeni said.
Administered every year
Dr Paul Yonga, a clinical epidemiologist and consultant infectiologist and tropical/travel medicine specialist based in Eldoret, speaking to Nation on phone about the findings, said the best option is to make a vaccine that covers all strains and to be administered every year.
“We will never be out of the woods when it comes to Covid-19 because scientists have not been able to measure T-cells or memory cells yet researchers found that T cells tend to recognise parts of Sars-Cov-2 that don’t mutate rapidly,” Dr Yonga said, explaining that T cells coordinate the immune system’s response and kill cells that have been infected by the virus.
He added that a mix-and-match approach to boosters would not work as well.
“It simply means one type of vaccine is used to prime the immune system to produce antibodies against a specific pathogen and, after some time, (between four and 12 weeks) a different vaccine targeting the same pathogen is used to boost a sustained production of antibodies against the pathogen.”
“The current strategy being applied in most, if not all, parts of the world is known as homologous prime-boost vaccination, especially with vaccines that require two shots.”
“Heterologous prime-boost vaccination is not something new in the vaccinology field as it has been applied in developing vaccines for infectious diseases such as dengue and influenza, albeit with mixed results,” Dr Yonga explained.
In June last year, Dr Francis Collins, a former director at the National Institute of Health (NIH), was of the view that a key issue a would be determining more precisely how long people exposed to Sars-Cov-2 will make neutralising antibodies against coronavirus.
While explaining that a vaccine that prompted the body to create more T cells against Sars-Cov-2 could help prevent disease caused by a wide range of variants, NIH funded a study that shows that the answer to this question will vary based on how an individual’s antibodies against Sars-Cov-2 were generated over the course of a naturally acquired infection or from a Covid-19 vaccine,” he said.
“The new evidence shows that protective antibodies generated in response to an mRNA vaccine will target a broader range of Sars-Cov-2 variants carrying ‘single letter’ changes in a key portion of their spike protein compared to antibodies acquired from an infection,” he said.





