Saving millions of lives one jab at a time
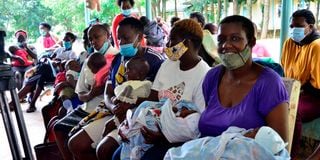
Mothers wait for their babies to be vaccinated at Yala Sub-county Hospital in Siaya County on April 19, 2021.
What you need to know:
- World Immunisation Week, celebrated in the last week of April, aims to highlight the collective action needed and to promote the use of vaccines to protect people of all ages against disease.
- The theme for this year's World Immunisation Week is “The Big Catch-Up” and aims to emphasize the need for countries to accelerate their progress towards ensuring that everyone, particularly children are protected from preventable diseases.
There is nothing more heartwarming than the sight of mothers seated on the bench outside a child welfare clinic hugging their chubby little babies as they await their turn to see the nurse. This is a picture that is replicated across the country, in all walks of life, whether it is in Naitiri Health Centre in Bungoma or in Kibandaongo dispensary in Kwale.
Once it is her turn, every mother knows the routine — the clothes come off, the baby is carefully laid on the weighing scale and the nurse charts the weight in the little purple book. This is followed by the administration of the oral vaccines, with the chubby cheeks being pushed together and the freezing cold drops quickly being dropped into the mouth. Finally comes the injections on the rounded little thighs, which make the baby realise that these two were up to no good! Mum quickly fumbles with the breast in an attempt to bribe the little one to calm down.
For decades, almost every mother in Kenya has observed this ritual faithfully without much thought to its origin. Even in the most remote parts of the country, she seems to have gotten this memo. A mother will walk miles to get her baby immunised. She may not understand the magnitude of this action, but it is her commitment that is certainly making the world a better place. To this end, the Healthy Nation brought together a team of experts to help us understand the world of vaccines better.
What are vaccines and how do they work?
Vaccines are biological substances that prepare your body to better protect itself when faced with the actual disease. It is typically prepared from an inactivated (killed) or weakened form of the actual disease-causing agent or from a part of its constituents or products. It may also be prepared from recombinant technology. It is used to stimulate the body’s immune system to be ready for attack.
Think of your body as a country and your immune system as the country’s defence forces. For one to build a formidable force, the recruits must be trained, drilled and transformed into tough soldiers ready for any eventuality, even if the war never comes.
The unvaccinated person’s immune system is like a fresh recruit to the defence forces. He is healthy and strong and capable of putting up a fight but has no skills or experience. When a pathogen (bacteria or virus) enters the body, the immune system generates antibodies to fight it off. The body has an uncanny ability to ‘remember’ the attack by retaining what is called ‘memory’ cells specific to this infection. That means that should the person fall ill again from the same pathogen, the memory antibodies that were created will recognise it faster, mounting a speedier and more efficient response, with the capability to subdue it better. This is the equivalent of the recruit going to war with no training.

Pupils from Melon Mission School in Nakuru County receive a Measles-Rubella vaccine during a past campaign.
However, in the defence forces, soldiers do not learn their skills at war. The recruit undergoes training geared towards transforming him into a skilled soldier who quickly recognises a threat and effectively neutralises it, with minimal impact on the civilians of the country, in this case, your normal body cells and organs. This training happens at boot camp, with conditions that simulate a real war for him to learn what to expect and how to respond.
Vaccines are our boot camp. They expose our immune system to the hostile conditions expected when the pathogen strikes and allow the system to prepare for an efficient and coordinated response, ready for when it will be needed. This is medically referred to as priming. Vaccines work to prime your immune system against future “attacks” by a particular pathogen. As a result, you gain future immunity against the disease without having to be sick.
Are vaccines always 100 per cent effective?
Vaccines are designed to generate an immune response that will protect the individual during future exposures to the disease. While we all have similar immune systems, individual differences determine how adequately a person’s immune system will generate a response. Hence some people may not generate adequately effective protection after vaccination.
With the awareness of these subtle differences, vaccines are tested to provide the highest effectiveness possible. Among the currently available vaccines for example, getting the prescribed two doses of the MMR (measles, mumps and rubella) vaccine results in 99.7 per cent of vaccinated individuals being immune to measles while it is 99 per cent after three doses of the inactivated polio vaccine.
Can the vaccines be combined in one injection and given once?
In Kenya, currently, the expanded programme on immunisations recommends vaccinating against 10 different disease-causing pathogens for a child under one year. The creation of the vaccine itself varies from agent to agent in line with the most effective preparation to trigger the immune system. Some are prepared as oral drops such as polio and rotavirus vaccines, while others are prepared as injections.
Further, some pathogens will require a single dose of vaccine for adequate coverage, while other pathogens may have different strains. These strains require that various forms of the same vaccine be given in order to achieve total coverage hence the need for multiple dosing given at specific intervals. All these considerations are the ones that determine the vaccine schedule and why it is not possible to package them all into a single shot. Currently, the shot combining the highest number of vaccines has six.
Can the baby’s immune systems handle so many vaccines?
Yes. Research shows that an infant’s immune system can handle receiving multiple vaccines at once even more than we currently recommend.
The immunisation schedule is based on infants’ ability to generate an adequate immune response to a vaccine as well as when the risk of certain illnesses sets in. The immunity passed on from a vaccinated mother to a baby in the womb provides temporary protection from some pathogens, which wanes with time. The baby must then be vaccinated to develop their own immunity by the time mum’s protection ends, such as measles at nine months. For pathogens against which mum is not able to pass on any protection, their vaccination is done early such as polio and hepatitis B given at birth.
What is the role of booster vaccines?
It is not completely understood why the length of immunity acquired from vaccination varies with different pathogens. Some vaccines offer lifelong immunity with only one dose, while others require boosters in order to maintain immunity. Disease progress is the period from the time a person comes into contact with the pathogen to when they show full signs and symptoms, right up until it heals, is cured or the person dies of it. Recent research suggests that the persistence of immunity against a particular disease may depend on the speed of disease progression. If a disease progresses too rapidly, the generation of the immune system’s memory response may not be quick enough to prevent infection. This is unless they’ve been ‘reminded’ about the disease fairly recently and are already watching for it. Hence boosters serve as a “reminder” to your immune system.
Can a vaccine cause the disease it is supposed to prevent?
If a vaccine has been made with killed versions of pathogens or with only a part of the pathogen, it cannot cause illness. With regard to live, attenuated (weakened) vaccines, theoretically they are capable of causing illness because they maintain some minimal capacity to multiply or mutate back into an infective form.

The tuberculosis vaccine fends off a slew of unrelated infectious diseases and its immune boost can protect newborns for more than a year. PHOTO | AFP
This very rare occurrence has been noted in some forms of the oral polio vaccine (OPV), leading to the increasing recommendation towards the inactivated form of polio vaccine (IPV). As a result of this risk, attenuated vaccines are not recommended for individuals with weakened immune systems such as cancer patients, transplant patients on steroids and patients with severe immunosuppression in AIDS. These individuals may receive a killed form of the vaccine where available. If not, the recommendation is to forego the vaccine altogether. Hence the need to ensure the vaccination of all those around them, to provide them with protection by proxy, what is medically known as herd immunity.
Despite this risk, live, attenuated vaccines generate longer-lasting immunity compared to the killed vaccines. Thus, killed vaccines are more likely to require boosters to maintain immunity. Killed vaccines, however, also tend to be more stable for storage purposes in addition to carrying zero risk for causing infection. Hence the need to find a safe and effective balance.
The Life Course Approach to immunisation
To many people, the concept of vaccination is regarded as a childhood affair and few appreciate their need beyond infancy. However, in health promotion, the application of the life course approach to an individual’s health and well-being means looking across one’s lifespan, from birth to old age or death.
Through this approach, we anticipate and provide for the holistic needs of an individual’s health and well-being, at various ages and developmental stages in life. With regard to immunisation, one is able to consider vaccines as needed through infancy (0-1 year), toddlerhood (2-3 years), pre-school (4-5 years), school going (6-9 years), adolescence (10-19 years), young adulthood (19-25 years), adulthood (26-49 years) and old age (50 years and above). It is this approach that has led to the recommendation of additional vaccines spread out over the lifespan.
The Human Papillomavirus (HPV) vaccine
HPV is the most common sexually transmitted infection even in monogamous relationships. The prevalence of HPV infection among women above 15 years of age ranges between 14 per cent to 51 per cent, depending on the region, and increases with age.
HPV infection may resolve spontaneously in approximately 90 per cent of individuals, but persistence of its presence in the body can cause genital warts and cancers of the anus, penis, vagina, vulva and back of the throat (oropharyngeal). The Human papilloma virus is the primary cause of 99.7 per cent of all cervical cancers, with two types — HPV16 and HPV18 — accounting for more than 70 per cent of cases.
Among Kenya’s 16.2 million women aged 15 years and older, at least 5,250 of them will be diagnosed with cervical cancer annually; of whom over 3,000 die. These deaths are easily averted if the country achieves 90 per cent immunisation coverage for HPV. The effectiveness of the vaccine is at its highest when given prior to HPV exposure, hence the rationale for vaccinating girls and women before their sexual debut.
There are three licensed HPV vaccines namely Bivalent Cervarix, which protects against types 16 and 18, the main cause of cervical cancer; Quadrivalent Gardasil vaccine which protects against types 6,11,16 and 18, widening the scope to protect against 90 per cent of genital and warts; and lastly, the Nanovalent Gardasil which protects against types 6, 11, 16, 18, 31, 33, 45, 52, and 58, that expands the protection to throat, head and neck cancers. These vaccines are produced through recombinant technology to yield virus-like particles, which do not contain any viral genetic material or any live biological product, hence they are non-infectious.
The recommended schedule of immunisation is based on the age group. For those aged 15 years and below, they receive two doses, given six months apart. For those aged 16 years and above, they get three doses given at zero, two and six months. Any woman or girl below the age of 45 is eligible for the vaccine even though the government is currently focused on vaccinating the primary target group of 10 to 14 years.
Vaccinations in pregnancy
The purpose of maternal immunisation is to protect both the mother and foetus from the negative effects of infections. Vaccination also provides the newborn baby with passive protection against vaccine-preventable infections acquired after birth.
In Kenya, it is recommended that pregnant women receive the tetanus vaccine; two shots are given at least four weeks apart, between 24- and 32 weeks gestation in the first pregnancy and then a single shot in the subsequent three pregnancies. This is the single most effective intervention that has almost eliminated neonatal tetanus in Kenya. The influenza vaccine, though not routinely administered in the country, is recommended in pregnancy.
Vaccines for special populations and their schedule modification
Due to specific medical conditions or high-risk exposures, some populations require specific non-routine vaccines for the necessary protection. These include people with chronic conditions such as sickle cell disease, rheumatic heart disease, and those who have had surgical removal of the spleen. The doctor will advise on the required vaccines over and above the routine schedules.
Other patients may require modification of the routine schedule to accommodate their unique issues. The vaccines may be delayed or withheld completely. These include premature babies, pregnant women, immunosuppressed people, HIV-infected people, diabetes mellitus, asthma, heart disease, liver disease and chronic kidney disease.
It is also recommended that certain professionals receive specific vaccines due to the risk involved in their line of duty. These include healthcare professionals, the disciplined forces, laboratory staff who handle biologicals and crew who serve on board luxury cruise ships.
Some vaccines are given in special circumstances to offer protection following certain exposures and incidents that may put individuals at risk of contracting life-threatening infections such as rabies vaccine for dog bites and tetanus vaccine following trauma or severe burns.
Outbreaks of serious infectious diseases such as cholera, Ebola and Covid-19 require vaccination as a key component of the emergency response measures employed to manage them. This protects both the healthcare providers and the populace, saving lives and minimising morbidity.
What are immunisation campaigns?
The Immunisation Agenda 2030 (IA2030) sets an ambitious, overarching global vision and strategy for vaccines and immunisation for the decade 2021–2030. For this reason, this year’s theme for World Immunisation Week fits right in: ‘The Big Catch-up’. In order to achieve this, the use of immunisation campaigns is employed to quickly reach large numbers with one or more vaccines.
They can be conducted at the national or sub-national level to meet the country’s objectives. The vaccines given may cover a single pathogen such as polio or measles campaign; or they may integrate multiple ones as required.
The campaigns may be Supplementary Immunization Activities, which deliver vaccination to all targeted individuals regardless of their vaccination status (prior history).
The aim is to rapidly raise population-level immunity and reduce the number of susceptible persons in order to achieve disease control or elimination.
Alternatively, they may be Periodic Intensification of Routine Immunization, where intermittent campaigns are undertaken to administer routine vaccinations to under-vaccinated populations. These happen during events like Child Health Days, Child Health Weeks, and National Vaccination Weeks. The vaccine doses provided here are part of the routine schedules.
Additional reporting by Dr Christine Chege, Dr Benjamin Elly, Dr Chris Barasa, Dr Ombeva Malande and Dr Conrad Wanyama