Vaccines through human history
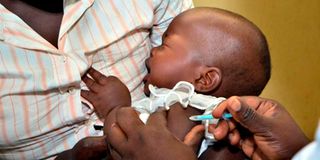
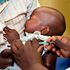
Seven-month-old Queensly Harriet receives her second dose of the malaria vaccine at Got Agulu Sub-County Hospital in Homa Bay County on April 16.
When the World Health Organisation (WHO) recommended the use of the RTS, S malaria vaccine among children in sub-Saharan Africa earlier this week, the region heaved with relief.
For decades, malaria has wreaked carnage in the tropical region, killing thousands of children every year.
WHO Director-General Tedros Ghebreyesus said “this is a historic moment. The long-awaited malaria vaccine for children is a breakthrough for science, child health and malaria control.’’
Communicable diseases have existed as long as man has lived on earth. Development of vaccines, though, has sometimes been a journey of equal parts frustration and patience, but also expensive both in terms of research endeavours and the lives lost during the wait.
From the Athenian pandemic in 430 BC to the Great Plague of London in the 1660s, the Spanish flu of 1918 and the current Covid-19 pandemic, epidemics have featured in the lives of humans for thousands of years, with varying degrees of severity and devastation.
Some pandemics have been regional and others global. Wherever they have swept, they have triggered social upheavals and ethnic suspicions, derailed wars and left a devastated population.
In medical circles, a pandemic is the gravest scenario when it comes to infectious diseases, dreaded by doctors and other healthcare practitioners – for obvious reasons. Pandemics spread fast, they evolve equally fast, have the highest number of casualties and often ransack healthcare systems.
Pandemic
To medical experts, containing a disease from exploding into a pandemic is a matter of priority. It’s for this reason that vaccines exist – to protect populations and to forestall public health catastrophes.
Sometimes, however, these horrors have been difficult to prevent. In Athens, for instance, the contagion killed two-thirds of the Greek city’s population. The Great Plague of London between 1665 and 1666 wiped out about 20 per cent of the inhabitants of the English metropolis.
The Black Death, though, is considered by historians the deadliest pandemic ever. When it struck Europe in the 14th century, it decimated the continent’s population by a third, killing between 75 million and 200 people.
So devastating was this pandemic that rotting bodies were scattered on European streets, preservation facilities too stretched and communities too overwhelmed to bury their dead.
France and England, who were engaged in war at the time, had to call a truce as the disease ran wildly out of hand. Not even the vikings could withstand its horrors as their excursions into North America were thrown off kilter.
Philip Slavin, associate professor in history at the United Kingdom’s University of Stirling says the Black Death puts Covid-19 “into humble proportions in comparison”.
So, how did man leave before vaccines were developed?
In her book “Life Without Vaccines”, social scientist Dr Margot Smith talks about how medical science has changed life in modern times by drawing comparisons with the 1930s when humans lived in dread of pandemics, but with few options.
The advocate for universal health care and economic justice recalls her childhood experience with rubella, and how she lay in bed in a darkened room for weeks. Her parents were convinced that light was bad for sick children’s eyes.
At the time, children with rubella were quarantined at home, missing school and other activities. But thanks to advancements in epidemiology and medicine, there are antibiotics and vaccines for rubella, and children need not lay at home.
Antibiotics
“I know survivors, men and women, who experienced illnesses before vaccines and antibiotics… some could not father children because they had mumps as children, a woman with a flail arm from polio, people with chicken pox scars, those deafened because of measles. I have friends who had polio then who now have post-polio syndrome that is, muscle weakness, fatigue and pain, for which there was no known cure,” she writes.
Throughout human history, some civilisations believed that pandemics were sent by God to punish those who disobeyed him. While people from Biblical times knew that diseases were contagious, knowledge on how these infections were spread was scanty.
When Louis Pasteur and Robert Koch found out in the 1860s that diseases were caused by germs, humanity had made a major breakthrough in the fight against diseases. This discovery would lead to a new world of medical exploration, and public health movement, laws and practices to control diseases, but also new fears on how epidemics originated.
Before the vaccines and antibiotics, people had invented ways of preventing spread of diseases such as quarantine and isolation of the sick.
“Quarantine was first used in Italy in the 14th century for ships that had visited places with epidemics. Later in the 19th century, it was a strategy to control the spread of cholera, yellow fever and smallpox,” Dr Smith writes.
Quarantine and isolation are being used today to control the spread of Covid-19.
In the olden days, one was required to quarantine for 40 days for polio and four weeks for diphtheria. For measles, four days were mandatory before the rash and four days after appearance of the rash. Rubella patients were isolated for seven days before the rash appeared and five days after the rash.
For chickenpox patients, two days were required before the rash and for six days until all sores developed crusts, while 21 days was the standard for whooping cough (pertussis) at the onset of a runny nose and other symptoms.
But which vaccine was the first to be developed in the world?
The smallpox vaccine was the first to be developed, according to historians. The disease killed about 30 per cent of patients and often left facial scars on survivors. In the 1790s, English physician Edward Jenner noticed that the faces of milkmaids were rarely scarred with smallpox.
The country physician found out that their exposure to cowpox, an infection of cows, protected them. This led to the development of cowpox vaccination for smallpox prevention –the word vaccine is derived from Latin, variolae vaccinae (smallpox of the cow).
After its eradication in many world countries, smallpox vaccinations are no longer required. The last naturally occurring case of smallpox was reported in 1977. In 1980, the World Health Organisation declared the world smallpox-free, and today, there’s no evidence of naturally occurring smallpox transmission globally.
The breakthrough in the smallpox vaccine and the identification of specific germs led to a search for vaccines for other diseases, whose discovery would protect millions of children around the world.
MMR vaccine
Later, a vaccine for polio, a disease that paralysed 75,000 children each year, was developed. Kenya last reported polio cases in 2013 when a large wild polio virus outbreak in Somalia led to an eventual importation of 14 cases to the country. Earlier this year, Kenya launched a door to door immunisation programme in 13 counties to tackle a polio outbreak after the virus was confirmed to be circulating in Garissa and Mombasa counties.
With vaccines available, countries globally, including Kenya, continue to update their immunisation programmes with the latest vaccines in the market. The MMR vaccine (for measles, mumps and rubella), DTaP vaccine (tetanus, pertussis and diphtheria) are given to children during clinic visits.
Before the development of an effective vaccine for rubella, 20,000 children were being born every year with brain damage in the 1960s while diphtheria killed more. Diphtheria was so terrifying not only because it could kill with stunning speed, but because it could hopscotch so easily from child to child by way of the coughing and sneezing it induced.
However, parents nowadays rarely know such grief because their children are protected by vaccines.
The level of protection has continued to increase year by year, with many more vaccines being developed including the “Haemophilus influenzae Type B (Hib)” and rotavirus.
According to vaccinologist Paul Offit, in the 1970s, Hib was a major cause of childhood meningitis, pneumonia, and sepsis (a systemic blood infection).
“Children with this bacterial infection came into the emergency room so routinely that the hospital maintained a special darkened room with a fish tank to calm the child while an anaesthesiologist rushed down and a surgical team prepared to operate.
“I had a lot of really painful conversations with parents when kids had meningitis or sepsis,” Dr Offit recalls. “Often kids would develop permanent hearing loss.”
However, with the introduction of an effective vaccine in the 1990s, incidences of Hib reduced.
Striking in 1918 when humanity was already distressed by World War I, the 1918 Spanish flu couldn’t have come at a worse time. Troops in the frontline were quite unlucky – if one survived enemy fire, they were more likely to die of the contagion.
The H1N1 influenza is believed to have killed about 100 million people as blunders by authorities, such as failing to impose lockdowns, fuelled its spread. But it’s the movement of soldiers during the war that’s believed to have accelerated its spread across the world.
Globalisation, urbanisation, war and other human activities, including farming and the attendant destruction of animal habitat, have been catalysts to the spread of pandemics. The occupation of countries by Western powers has often coincided with pandemics.
One year after Fiji became a crown colony of Britain in 1874, for example, the measles pandemic hit, wiping out 40,000 inhabitants of the South Pacific nation.
During the hunter-gatherer days of humanity, however, the occurrence of pandemics was nearly non-existent. At the time, humans lived in more loose societies, moving from place to search in search of game and edible plants. This lifestyle of constant mobility significantly curtailed the spread of diseases with the potential to become a pandemic.
When humans started practising farming during the agrarian period (about 10,000 years ago), there was plenty of food for everyone, which allowed humans to settle and live in communities.
While food security had been realised, this communal living became a catalyst for the spread of diseases. Infections could spread faster and affect more people than ever before.
Medical historians believe that tropical diseases such as malaria, influenza, cholera and tuberculosis were first recorded after humans started practising agriculture and living in settlements such as towns and villages.
Bacteria
Officially known as Hansen’s disease, leprosy – a disease that causes physical deformity – had been around for many years, but it would escalate into a pandemic in the Middle Ages in Europe.
About 200 years ago in the 1810s, the first cholera pandemic, suspected to have originated from Russia, emerged. The disease, which spreads through water and food contaminated with faeces, has recorded the highest number of pandemics at seven.
During Britain’s occupation of India, which began in the late 1850s, British soldiers are said to have carried the bacteria to the subcontinent. In a country that was still densely populated (150 million), the bacteria spread fast.
Even after the first cholera vaccine was developed in 1885, nearly 70 years later, its rampage wasn’t halted. For the next 150 years, the disease would continue to devastate the world. Cholera casualties run into hundreds of millions worldwide.
There have been other proportionally ‘‘smaller’’ pandemics by comparison, with fewer casualties, such as the Russian flu of 1889 (360,000 deaths). While put into context, however, their impact was horrendous.
At the time of the measles pandemic in Fiji, for instance, the country had slightly over 120,000 people, which means a third of the population was taken down by the disease.
Until Covid-19 broke out 23 months ago, HIV/AIDS was considered the deadliest pandemic in the world. First discovered in 1981 among gay couples in the US, Kenya recorded its first case in 1984.
For the next 15 years, thousands would be infected and die as Kenyans lived in dread of contracting the virus. The disease would also inspire all sorts of myths, from the absurd to the outrightly bizarre, as people sought to understand its devastating nature.
The world is still waiting for the first HIV vaccine.
HISTORY OF VACCINES GLOBALLY
1706: Africans use variolation (deliberate infection) which made people assume they were immune to smallpox
1721: 3 per cent of case fatalities as a result of variolation
1796: First successful vaccine (smallpox) by Edward Jenner. In 200 years, the vaccine underwent medical and technological changes and eventually eradicated the disease
1802: Dr Jean de Carro encouraged vaccination and discouraged variolation
1803: Origin of the term vaccination. Edward Jenner insisted that the term vaccination be credited to Richard Dunning. It came from the Latin word for cow, ‘vacca’
1885: Rabies vaccine used in humans
1885: Development of a live attenuated (severity reduced) cholera vaccine by Ferran Jaime
1896: Basis for typhoid vaccination established
1904: Anthrax vaccine
1935: Early polio vaccine trials
1936: Yellow fever Vaccine developed
1945: Influenza vaccine approved
1948: Vaccine for both diphtheria, tetanus and pertussis (DTP) introduced
1955: Polio vaccine results announced; found to be 80-90 per cent effective against paralytic polio
1958: First measles vaccine is tested
1974: WHO includes BCG in the list of vaccines
1974: Chicken pox virus strain attenuated for vaccine
1978: Kenya was part of the Alma Ata World Health Assembly declaration that launched expanded programmes on immunisation in many parts of the world.
1980: Rabies vaccine produced
1987: Conjugate Hib vaccine licensed
1989: Oral typhoid vaccine licensed in the US
1999: Rotavirus vaccine withdrawn
2006: Rotavirus vaccine recommended
2006- HPV vaccine licensed in the US
2006: Hepatitis A vaccine recommended for all children
2010: Meningococcal vaccine rolled out in Africa
2020: Kenyan government approves human Covid-19 vaccine trials
2021: Covid-19 vaccines become available. Malaria vaccine, Mosquirix, approved for use by WHO, Kenya was one of the countries that led the trials.