With this procedure, surgery doesn’t have to be nightmare
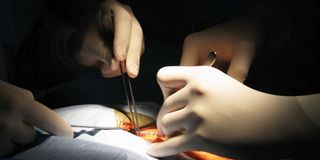
Laparascopy has changed the way surgical procedures are done. It allows a surgeon to access the inside of the abdomen and pelvis without having to make large incisions in the skin. PHOTO | FOTOSEARCH
The worst news a patient can probably get is that a doctor has tried everything to treat their condition and the only way out is a surgery.
Surgery is usually associated with pain, high costs, lengthy hospital stays and long recovery journeys. For women who find out they have fibroids, hearing they might have to undergo surgery, for their lives to go back to normal, is usually a nightmare.
Recently, there have been many advances in health technology and one of these is laparoscopy, also known as keyhole surgery, which has saved such patients the trouble of a complicated surgery.
LESS INTRUSIVE
NHS defines laparoscopy is a surgical procedure that allows a surgeon to access the inside of the abdomen and pelvis without having to make large incisions in the skin. This surgical technique enables patients to be up on their feet and out of hospital sooner than expected, because it is less intrusive.
Globally, laparoscopic surgery has been around since the 1980s. However, not many hospitals in Kenya have the equipment and expertise to conduct such procedures.
Before June 27, 36-year-old Doreen Ongoro had suffered untold pain. “It was terrible,” she tells HealthyNation. Laparoscopy changed her story. “Before the procedure, I had several clinics to assess my situation and when the doctor told me that I had fibroids, he advised that it was best to have them removed,” says Doreen.
No medication could suppress the fibroids. She would have heavy periods and a strikingly painful backache.
She is not new to a surgery room, as a patient, having undergone a caesarean-section 10 years ago. The CS was an open surgery, which is quite different from a laparoscopic surgery.
“The laparoscopic surgery is less invasive and less painful and the healing process is a bit faster than the open surgery I had when I got my baby. I got the surgery and went back home the same day.
She also did not have to go back to hospital for any post-surgery complications. Even better, her periods are neither painful nor heavy.
Jane, 25, who requested anonymity, had ovarian cysts that had grown out of proportion and needed to be removed urgently. “My condition started some time in February. Then, my periods extended from the normal three days to over a month,” she recalls.
On May 30, at 6.30am, she was in hospital ready for a laparoscopic procedure which, she says, took about an hour-and-a-half. She regained consciousness after four hours and the pain that had been bugging her had gone. She went home the same day.
MINIMAL TRAUMA
The two patients make Dr Bob Achila, a gynaecologist at the Aga Khan University Hospital, a happy man. He is one of the doctors in Kenya that has received extensive training on laparoscopy. “Laparoscopy is a minimal access surgery that has revolutionised gynaecology,” he says.
The advantages outweigh the disadvantages, he adds. Patients generally have fewer complications. “If the government were to adopt this kind of technology in public hospitals, it could help alleviate the problem of congestion since it drastically reduces the duration of hospitalisation with many patients being able to go home the same day, says Dr Achila.
He says patients are able to go back to normal activities faster than after traditional open surgery since there is “minimal trauma and a meticulous handling of tissues during operation”.
For conditions like endometriosis, he says they can be directly visualised by laparoscopy, and that it is a great diagnostic tool. “Pregnant women can have the procedure done on them, just not for C-section, but pregnancy complications like ectopic pregnancy – when a baby develops in the fallopian tube rather than the womb. It is a life-threatening situation that can be successfully treated using laparoscopy,” says Dr Achila.
Other operations done by laparoscopy include appendectomies- removing of the appendix and cholecystectomy- removal of the gallbladder.



