In Kenya, contentious malaria drug is seen as a lifesaver
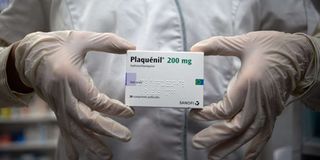
A box of Plaquenil, an anti-malaria drug hydroxychloroquine made by Sanofi, used for years to treat malaria and autoimmune disorders. To date, no clinic trials have demonstrated a real effect on the Sars-Cov-2 virus. PHOTO | AFP
On one sunny Wednesday morning at the Afya House parking lot, the Ministry of Health officials unveiled a huge consignment of essential medicine from the Indian government.
The drugs from India included antiretroviral drugs as well as hydroxychloroquine, a drug that has long been used to treat malaria as well as other conditions such as lupus and arthritis.
Hydroxychloroquine is a molecule derived from chloroquine. It' is used to reduce fever and inflammation, and the hope has been that it can also inhibit the virus that causes Covid-19.
Some early studies showed that it may be able to shorten the duration of symptoms experienced by coronavirus patients, while others indicated it had no positive effect at all. Kenya put in a special request to India and was allowed to import hydroxychloroquine from the country.
EMERGING EVIDENCE
Health Chief Administrative Secretary Rashid Aman said Kenya imported the drug to be used in clinical trials that will be conducted in the country. He said that should the trials be considered a success, the drug would come in handy.
Kenya is part of the “solidarity” international clinical trial launched by the World Health Organization (WHO) and partners to help find an effective treatment for coronavirus. More than 400 hospitals in 35 countries are participating in the Solidarity Trial, which involves thousands of patients.
The trial will compare four treatment options against the standard of care, to assess their relative effectiveness against coronavirus.
By enrolling patients in multiple countries, the trial aims to rapidly discover whether any of the drugs slow disease progression or improve survival. Other drugs can be added based on emerging evidence.
A few weeks after the importation of the drug, however, concerns were raised over the efficacy of hydroxychloroquine around the world, and WHO paused the drug study so the trial’s data safety monitoring board could analyse the results generated so far and see if any safety concerns were apparent.
Although the WHO resumed clinical trial exploring whether hydroxychloroquine can effectively treat Covid-19 this week, there are concerns as to why the drug’s safety and efficacy issues are only raised now yet Africa has used the drugs for decades to treat malaria.
On her Twitter page, Rebecca Enonchong, a Cameroonian born technology entrepreneur and also the founder and CEO of AppsTech, said: “Funny how when the drug was being administered to millions of Africans as a malaria drug, these risks didn't seem to bother anyone.”
IRREVERSIBLE BLINDNESS
Here in Kenya hydroxychloroquine, a molecule derived from chloroquine is used in patients with autoimmune diseases such as lupus while chloroquine was used for decades as a cheap and safe drug against malaria, although their effectiveness in this field is now undermined by growing parasite resistance. The drug is known to have serious side effects, including muscle weakness and also affects the rhythm of the heart.
In Africa, chloroquine has always had the reputation – wrongly, according to its advocates – of being especially toxic. In the 1970s it was often used in suicides. Besides, it has known toxic effects on the retina, particularly when it is taken long term.
The Pharmacy and Poisons Board (PPB) recently stated that the risks from self-medication from hydroxychloroquine and chloroquine were largely rooted in illegal sales further warning pharmacists against selling it without prescription.
In a memo, PPB CEO Fred Siyoi said there had been a rush to buy chloroquine and hydroxychloroquine which are prescription-only drugs. He said the use of hydroxychloroquine without prescription may lead to irreversible blindness.
Chief executive officer of the Pharmaceutical Society of Kenya Daniella Munene said the drug is not used for malaria anymore in the country and is currently used on patients with autoimmune diseases. “Most people in Africa and parts of Asia developed resistance to the drug and so it is now used for people who have conditions such as lupus here in Kenya. It affects the rhythm of the heart and doctors only subscribe to it patients after assessing the patient’s heart,” said Dr Munene.