Eastern Africa can turn the tide on visceral leishmaniasis: Here's how...
Sponsored by FIND
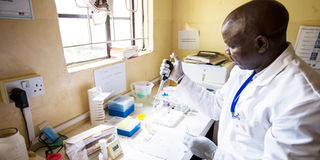
Conducting rapid tests in Kenya.
By Joseph Ndung’u
In Eastern Africa, some estimates suggest that tens of thousands of people contract visceral leishmaniasis (VL) each year. The region has the highest burden of this serious neglected tropical disease in the world.
VL, which can cause life-threatening damage to internal organs, is the most severe of a group of diseases caused by Leishmania parasites. Infection begins when a female sandfly, carrying the Leishmania parasite, feeds on a human being. The parasite then enters the bloodstream. Symptoms include fever, weight loss, and an enlarged spleen or liver. Without medical intervention, this disease is fatal in more than 95 percent of cases.
A combination of factors make certain communities more vulnerable to this parasite’s effects. For example, regions suffering from food shortage caused by drought and other effects of climate change, will in turn have greater levels of malnutrition. People suffering from poor diet may have an increased likelihood of becoming acutely sick. Armed conflicts have destroyed housing and infrastructure in some countries, leaving communities at greater risk of contracting VL from the bite of the sandfly, which transmits the disease.
The disease is curable, but only if caught early and properly treated. That can be a challenge because VL primarily strikes in remote, rural areas. Many affected communities are far from healthcare services.
Fortunately, the tide against VL could be turning. In recent years, Kenya has made steady progress in addressing this disease. In fact, it could become the first country in Eastern Africa to achieve elimination of this public health problem.
At the core of this effort, Kenya’s Ministry of Health has put emphasis on innovative diagnostic approaches. To eliminate VL, Kenya, along with the support of partners such as FIND – the global alliance for diagnostics – is taking critical steps to better identify, treat, and monitor infections.
Kenya is taking an innovative approach by enabling health professionals to go out and proactively test people, rather than waiting for them to present at health facilities. This shift is modelled in part on how other countries, such as Uganda and Côte d’Ivoire, have successfully eliminated another neglected tropical disease – sleeping sickness – as a public health problem.
As part of this effort, Kenya is strengthening healthcare facilities and personnel knowledge. To identify VL, healthcare workers need to use several diagnostic tools. Rapid diagnostic tests that can be conducted anywhere, without need for electricity or any other health infrastructure, offer a powerful first step.

Testing patient samples for VL as part of a clinical trial in Kenya.
When a sick person presents with symptoms suggestive of VL, these easy-to-use tests identify blood proteins that indicate someone may indeed have a VL infection. A combination of strong clinical signs and a positive rapid test are often adequate for a patient to be put on treatment. Additional specialised diagnostic tools to confirm a diagnosis are also available. A patient confirmed to have VL requires hospitalisation and specialised care.
Kenya’s Ministry of Health, with the help of partners, has therefore taken steps to acquire and distribute essential diagnostic equipment. By ensuring that more health centres in counties where the disease is found perform rapid diagnostic tests, for example, people throughout those counties can access screening for VL, closer to home. Along with these diagnostic instruments, training healthcare workers is vitally important. Personnel at facilities throughout the affected counties need to know how to use the available diagnostics, how to treat patients, and where and when to refer people to other healthcare providers.
In many remote healthcare settings, an added challenge is personnel turnover. Rather than start from scratch with new trainings for each group of staffers, training now incorporates skills that allow health workers to train one another. That added step ensures lasting knowledge within Kenya’s healthcare community.
By building up the capacity and expertise of Kenya’s facilities in these ways, the country is creating a better network of specialised responders. If someone living in a remote area starts to show symptoms, they are more likely to find a centre that, at minimum, offers a rapid diagnostic test. Then, if need be, that centre can connect them with a specialised facility for follow-up testing and treatment.
The expanded healthcare network may also address a second hurdle in controlling VL’s spread. After treatment, some patients develop skin lesions. This condition is not fatal, but individuals with these lesions may, in turn, infect sandflies. These insects then spread the disease further. In principle, the best safeguard against this problem is for people to return to medical care if any lesions appear. But in practice, issues like cost and distance deter many from doing so. Efforts that improve access to healthcare facilities and specialists could address this problem.
More broadly, the Kenyan Ministry of Health is taking steps to educate the public and healthcare volunteers. People living in counties where VL is present need to learn about this disease, how to spot its symptoms and what to do if infection strikes.
Taken together, these efforts are empowering communities, volunteers, and health workers alike. With earlier detection and treatment a top priority, this devastating disease can ultimately join sleeping sickness in being consigned to the history books.
Professor Joseph Ndung’u is Executive Director of FIND in Kenya


