New polio vaccine will only be available in special circumstances: Kenyan expert
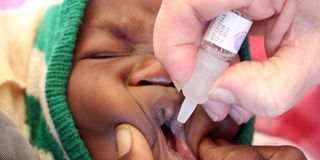
A child receiving a polio vaccine. A new vaccine that has the potential to shield against outbreaks caused by a mutated polio strain will only be given under special conditions.
A new vaccine that has the potential to shield against outbreaks caused by a mutated polio strain linked to the oral vaccine has received an emergency listing from the World Health Organisation (WHO).
Unlike routinely used oral polio vaccines, this particular one, known as Novel Oral Polio Vaccine Type 2 (nOPV2), is a highly controlled type of vaccine that will only be available for specific response activities, said Dr Peter Borus, who heads the Kenya Medical Research Institute (Kemri) polio laboratory and is a WHO lab scientist.
The vaccine was introduced as part of the global endgame strategy against the wild polio virus, which can cause paralysis among those infected, mostly children. To stamp out vaccine-derived polio outbreaks, the WHO granted emergency use listing (EUL) for the new oral polio vaccine on November 13.
Wild polio-free
In August last year, Africa was declared wild polio-free after three decades of campaigns against the disease that once paralysed about 75,000 children on the continent every year. Although most continents in the world have managed to get rid of polio, there is growing fear that the current vaccine used to guard against the disease could spark a new outbreak.
To completely eradicate the debilitating disease in the world, scientists have been gunning to replace the vaccine, which contains a weakened version of the poliovirus, with one that cannot mutate and regain abilities to cause an infection.
“Particularly in areas where vaccine coverage has been very low, we still have been having a problem in the sense that during outbreaks, a small percentage of the poliovirus type 2 has been reverting back to virulence,” explained Dr Borus.
Modified version
The nOPV2 vaccine is a modified version engineered to guard against poliovirus type 2, and scientists argue that it has an improved genetic stability, making it less likely to mutate and revert into a form of the virus that can cause infection and paralytic disease. It was developed by Bio Farma, an Indonesia-based vaccine and serum manufacturer.
Following elimination of the virus in many parts of the world, the response has been to cut out the strains that become reactivated by coming up with a vaccine that is more genetically stable, said Dr Borus.
“This is what we are calling the nOPV2 vaccine,” he said in an interview with the Nation.
Although the vaccine is the first of its kind developed to protect against a mutated form of the poliovirus that is causing disease outbreaks across Africa and Asia, it is not the first time a global switch of a polio vaccine is taking place. In April 2016, following the eradication certification of type 2 polio, countries using trivalent oral polio vaccine (tOPV) implemented a global switch to bivalent oral polio vaccine (bOPV), which protects against polio types 1 and 3.
Using the new vaccine, the scientist noted that in a small group of people in stringent conditions of containment, the problem of vaccines reverting to virulence and causing the disease will no longer happen.
Prevents transmission
Unlike inactivated polio vaccine (IPV), which primarily protects the person vaccinated, OPV protects the individual as well as prevents transmission to others. But since the vaccine uses a weakened or “attenuated” version of live poliovirus to elicit an immune response, it carries with it a miniscule risk of getting reactivated and causing an outbreak in regions with low immunisation coverage. Remnants of the live virus can be shed from individuals recently vaccinated with OPV and in turn circulate back into the environment, and eventually cause infections among susceptible individuals.
“Mucosal immunity, which is very crucial in poliovirus immunity, cannot be given by IPV, but an OPV, which cannot change and revert back to virulence and that is why this novel oral polio vaccine 2 was developed,” said Dr Borus.
Though rare, if this transmission goes on long enough in under-immunised populations — usually about 12 to 18 months — the weakened virus can genetically change and revert to its virulent state, giving rise to what is called “circulating vaccine-derived” poliovirus. Type 2 is currently the most prevalent form of the vaccine-derived virus.
Immunisation disparities
Despite years of progress in improving immunisation coverage nationwide, Kenya still faces enduring subnational disparities, with the government estimating that about 600,000 children are missing out on even a single dose of either BCG, measles and three doses each of OPV and pentavalent, pneumococcal vaccines. These gaps may be exacerbated by the disruption of some vaccination services under the pandemic.
Dr Borus also said Kenya will only have the new vaccine in the event of a vaccine-derived polio outbreak.
Not routine immunisation
“[The] nOPV2 is not given in routine immunisations, you cannot go to a clinic and say you want it,” he said.
There is also a long process of acquiring it, which involves assessing risks and regulatory bodies that have to ensure there is a plan in place so that once the vaccine is administered, what is left is completely taken out and removed from the system.
The vaccine received the WHO greenlight following new research published in two papers in The Lancet and Phase 2 trials of 1,200 healthy adults, young children, and infants suggest the new poliovirus vaccine may have the potential to overcome outbreaks caused by a mutated polio strain linked to the oral vaccine that typically circulates in areas of low immunisation coverage, and poses one of the biggest barriers to eradication.