Thousands at risk as malnutrition numbers in refugee camps soar
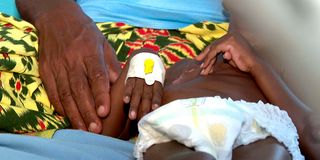
Khalid Ali Alkadir, who is malnourished, at a hospital in Hagadera Refugee Camp, Dadaab,Garissa County on July 24
What you need to know:
- According to data from Unicef, the nutrition situation among children in Garissa County remains critical; with over 60,000 children suffering from malnutrition and 17,000 others severely malnourished.
- A survey carried out in 2019 on the nutrition situation in Garissa shows that it is critical at phase three, with global acute malnutrition of 19.6 per cent. As a result, WHO has designated Garissa among other counties as an acute food and livelihood crisis area.
Thin, bloated bellies. Protruding ribs. Pale and dry skin. These were the images of crying babies at the Hagadera malnutrition ward in Dadaab, Garissa County, when the Healthy Nation team visited the refugee camp.
It is a landscape of desperation.
The oddly thin arms of many children at the camp stand out.
A silent crisis is unfolding.
The innocent faces that should radiate with youthful energy are marked by hollow eyes and inactive expressions.
At the heart of the camp where a hospital is situated, a number of wards are crammed with malnourished patients; old, young, youths and expectant mothers. The paediatric ward handles more children than its required capacity of 30 patients. About 50 children are admitted at the ward.
Beyond the statistics and figures lies a poignant narrative of lives caught up in a vicious cycle of poverty, inadequate access to nutrition and the rush for safety from the neighbouring Somalia.
The Healthy Nation team sheds light on the complexity of their struggles and the urgent need for a call to action.
At the age of five, like his age mates, Khalid Alkadir is expected to be playing around but his frail look won’t allow him.
Alkadir was admitted to hospital last month at a time his system was shutting down. At the age of five, he weighs four kilogrammes, way below the expected 25 kilogrammes for children his age. He is suffering from acute malnutrition.
He does not have proper meals and only feeds on porridge in the morning, which is prepared from donations given by the World Food Programme. The family eats one meal a day.
In April, the family joined a new wave of Somalis on the run. They came when the infant had already developed hydrocephalus and because his family is not yet registered as new arrivals, they depend on their nephew at the camp to survive. Hydrocephalus is a neurological disorder caused by an abnormal build-up of cerebrospinal fluid in the ventricles deep within the brain.
“This has actually worsened the situation. I am joining my nephew, who has a family of 10. I have seven children. In total, we are 19. Imagine cooking teo kilogrammes of rice for the whole family. Would that be enough? Asked Ali Hassan, Alikadir's father.

Ali Hassan, Khalid Ali Alkadir’s father, during the interview.
In the morning when the flour is available, the family prepares porridge, if not they eat what is available and in most circumstances, they go without food.
“Even eating little to give him energy is a task, he can’t eat solid food and he can’t walk. I am afraid my son is dying,” his father laments at the hospital where they are currently admitted.
He says it is not easy to get milk daily since he does not have money and the family is not a beneficiary of what other refugees are given at the camp.
“The fact that he does not eat only aggravated his condition since there is also nothing to feed him. In most cases, a child is more susceptible to infection and illness when they do not feed or eat enough. The more they lose weight and become malnourished,” said Dr Silas Chirchir, who is in charge of International Rescue Committee (IRC) at Hagadera Refugee Camp.
Alikadir’s family’s situation is a representation of many families at the refugee camp who are now suffering from malnutrition. The situation, according to the experts, has been worsening every year.
Dr Chirchir says drought in Somalia has worsened the situation at the camp, with many who are already in a bad state fleeing Somalia.
“The situation that we are seeing here at the hospital is worrying. Most of them are fleeing when they cannot even talk. There is nothing to eat,” Dr Chirchir said.
He noted that malnutrition is categorised as at risk, moderate and severe, and each category is handled differently. At the hospital, there has been an upward trend in all the wards, with expectant mothers and children being the most affected.
The under-five are the most affected because their immunity is compromised. For this group, nutrition is vital. However, many families now survive on a diet of black tea and porridge.
In July, the Hagadera hospital recorded 400 patients who were malnourished compared to last year when 347 patients were admitted for malnutrition.
“For the last two weeks, the hospital has been busy and we have had to transfer some patients to Garissa Referral Hospital, with many of them being severely malnourished,”
Given the humanitarian work of the IRC, it has come up with a single therapeutic approach to treat the patients, which is community-based.
“Those admitted at the hospital are just but a few. At the community level, many are dying in silence more so the new arrivals, who are not yet registered and do not have what to eat,” Dr Chirchir told Healthy Nation.
However, with the help of the community health volunteers, they have been able to administer a single therapeutic product, which the families take at their homes.
Malnutrition, according to the World Health Organization, occurs as a result of faulty nutrition or when foods consumed lack basic nutrients of vitamin. Starvation can also contribute to malnutrition.
“It develops when the body does not get the right amount of nutrients, minerals or vitamins needed to grow and to maintain healthy functioning of organs,” Dr Chirchir explained.
The symptoms are sudden loss of weight, dry skin, pale and with rashes, tender bones and general body weakness. Other people may have thin hairs that can be pulled out with ease and with occasional bleeding from the gum.
“Severe malnutrition can kill. Left untreated, prolonged malnutrition causes the body to lose its stock of carbohydrates, fats and proteins. The organs including the brain and the heart start to struggle,” Dr Chirchir said, adding that if the current situation at the camp is not dealt with urgently, more lives will be lost.
At the L6 health post at the camp, women are lining up ready to pick super cereal plus fortified corn soya blend flour that is given monthly as a preventive and treatment measure for malnourished mothers and children.
Before one is given the flour, their weight and measurements are taken to see whether they are improving or worsening.
It is Binto Mahat’s turn to step onto the scale. She still weighs 42 kilogrammes. She is seven months pregnant, but with nothing to feed on.

Binto Abukar Mahat,an expectant mother who is also malnourished, walks home after receiving her food portion on July 24 in Hagadera Refugee Camp.
When her mid-upper arm circumference (MUAC) measurement was taken, the reading fell on the red code, reading 18 millimetres, indicating severe malnutrition. The MUAC is a common measure for malnutrition.
The band with millimetres reading is coded in different colours. A measurement in the green zone means the child is well fed, yellow means the child is at risk while the orange zone means the child is moderately malnourished.
When a mother is severely malnourished, they are given four packets of the flour to take for a whole month while those who are pregnant and are at risk of malnutrition are given two.
In the morning before coming to pick the flour at the facility, Mahat tells us that she had a cup of black tea and a piece of “anjera”(Somali form of chapati).
When Healthy Nation caught up with her around at her shelter of branches and plastic sheeting, she was eating a raw mango and salt.
“I know I am losing weight every day because I do not eat well or eat a balanced diet. It pains me that last month (June), I weighed 45kgs but this month (July) it dropped to 42 kilogrammes. The same was witnessed in my first child,” she said.
Even with the flour that she is given, with the strict instruction that it is for one individual, she still shares it with her family members.
Families skip meals and sleep early to escape the gnawing in their stomachs. They hide bony faces and emaciated bodies in voluminous black robes and veils.
Angela Kiprop, senior nutritionist officer with the IRC, said most of the malnourished cases both in the community and in the hospital are caused by poor feeding habits. Most of them feed on carbohydrates. They mostly take ugali, porridge and black tea.
“They eat the same food every day but the food has zero nutritional value. This is why the numbers are not looking any better.”
She added that the trend in the number of malnutrition admissions for expectant mothers and under five is worrying.
In January, there was an upsurge, with 83 children suffering acute malnourishment admitted at the stabilisation centre. In February, March and April, there was a decrease ; with 40 children per month being admitted. In June, the camp recorded 66 cases.
“In May, 96 children sought admission. This was because many had diarrhoea and did not have food at home,” said Kiprop.
In the programme, there are 1,253 active cases of moderately malnourished children and 283 mothers being moderately and severely malnourished.
She attributed the upsurge to food rationing. According to a survey conducted in March, Hagadera camp had a total of 145,418 people, with funder- five population of 20,197 and new arrivals still coming to the camp.
According to data from Unicef, the nutrition situation among children in Garissa County remains critical; with over 60,000 children suffering from malnutrition and 17,000 others severely malnourished. A survey carried out in 2019 on the nutrition situation in Garissa shows that it is critical at phase three, with global acute malnutrition of 19.6 per cent. As a result, WHO has designated Garissa among other counties as an acute food and livelihood crisis area.
The 19 per cent figure is above the emergency threshold, which is 15 per cent, according to WHO. The severity of malnutrition is only acceptable if the prevalence is less than five per cent.
Ms Sarah Borchers, who works at the World Food Programme in Dadaab Refugee camp, said the rationing of food will worsen the situation.
Last year, the refugees were getting a food ratio of 80 per cent. But funds ran out and from July, the ratio was reduced to 60 per cent.
“This means that we have to cut down on the cereals that are being provided to them as well as nutritional products This is not ideal, we would really wish to give 100 per cent, but this is not possible.”
She explained that the effects are already being felt since the nutritional status of children at the camp is wanting. The WFP provides monthly food assistance to 360,000 refugees who have largely come from Somalia.
In addition to those registered at the camp who are already getting food assistance, there are new arrivals and they are sharing the little that they are given among themselves.
“The Somalis have a sharing culture and for those who have not been registered, they do not get the food assistance. So they share the little they have among themselves.”
Ms Borchers said she is working with partners to ensure that the new arrivals are registered as fast as possible so that they benefit from the food aid.
Also, once they are registered, apart from the in-kind food assistance, they also receive electronic cash transfers dubbed, “Bamba chakula”. In the month before this interview, for instance, each person received Sh850, but this has since reduced to Sh450.
“The money was to cushion the starving families and help them buy nutritious food that is not provided by the WFP. But with the reduction of the money, the nutritional situation for many people will worsen,” she noted
Ms Borchers made an appeal to donors to disperse funds, which are essential to addressing the high requirements for protection and life-saving assistance. “I am requesting our existing donors to step up and give more. I am requesting the world not to forget us. It is easy to forget about a refugee but when you meet the families here, seeing people who have just arrived with really desperate nutritional and health status, you can tell that they need help. This is about saving lives,” she appealed.
Already, with the reduced funding for over a year now, Kenya has reported a shortage of ready-to-use therapeutic foods used to fight severe acute malnutrition.
The peanut-like paste fortified with proteins and vitamins known as Plumpy'nut could be the difference between life and death for thousands of children.
The shortage of life-saving medical products is due to Kenya’s reclassification as a low-middle-income country in 2014. It was previously classified as a low-income country. This new status means the country is capable of buying some life-saving products such as Plumpy’nut and, as a result, donors withdrew their support.
Even with the change in the country’s status, is it in a position to take care of its malnourished population? The Ministry of Health lists therapeutic foods as part of essential medicine procured by the Kenya Medical Supplies Authority and distributed to counties.
Globally, Unicef is the world’s largest buyer of therapeutic food, procuring 80 per cent of the world’s emergency supplies and supplying it to health facilities in Kenya enough to provide a child with six weeks’ worth of the therapeutic food until the child is nourished back to health.





