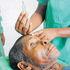
Martin Imbalambala, former AFC Leopards captain and Harambee Stars midfielder, during the interview at Makadara Football Grounds in Nairobi on August 16. He went blind in 2018.
| FRANCIS NDERITU | NATION MEDIA GROUPHealth
Premium
Martin Imbalambala: I went to bed with a headache and woke up blind
What you need to know:
- Martin was referred to Lions SightFirst Eye Hospital in Loresho, Nairobi, where doctors established that he was battling glaucoma.
- According to the Ministry of Health, glaucoma is a group of diseases that gradually affects the optic nerve.
- It is the second leading cause of vision loss globally and it continues to pose a challenge to eye health professionals in the country.
Imagine going to bed one evening and waking up the next day unable see again, forever.
For Martin Imbalambala, former AFC Leopards captain and Harambee Stars midfielder who once had a dream to play in the English Premier League, 2018 is the year he will live to remember.
The 33-year-old, orphaned at an early age, hails from Kisatiru village in Vihiga County.
He tells Healthy Nation it happened one Thursday in September five years ago after an intense day of football training.
“On that day, I went for training early in the morning and was out by 2pm.When I got home (in Eastlands, Nairobi) at around 5pm, I started having a severe headache, compelling me to take some painkillers with the hope that the pain would subside before dinner,” the father of three narrates.
He had been training in the rain and thus thought the headache was related to some fever. But he had been training under such weather conditions since his days at Chavakali High School.
By 9pm that night, the headache became more intense. Martin took more painkillers and decided to sleep it off.
“By 3am, my entire body was in pain, the pain had now taken to my eyesight and the headache had culminated into a never-ending migraine, which made sleeping impossible,” Martin recalls.

Moses Imbalambala, a former footballer, engages young boys after a practice session at Makadara Football Grounds in Nairobi on August 16.
He says at around 6am the pain had disappeared. He woke up and asked his wife to switch on the lights. “I was shocked when she told me the lights were on . We really argued because all I could see was total darkness,” Martin says. “I asked her to hand me my phone. I could feel it vibrate but couldn’t see it.” Martin had lost his eyesight.
From his balcony, he could hear people chatting outside but he couldn’t see them. “I could feel the sun shine on my face but I couldn’t see the rays.”
He was speechless and sat alone staring blankly into the darkness that had shown up in his life as tears rolled down his cheeks.
Martin called his brother who helped his wife rush him to Thika Level Five Hospital. “After a series of tests, doctors told me that they had not noticed any issue with my eyesight.”
They gave him an injection, assuring him that he would be able to see again after 30 minutes. “But to date, I am still waiting for those 30 minutes to elapse so I can see again,” says Martin.
The doctors hospitalised him for one month and then put him on medication. They gave him 12 tablets in the morning and 12 in the evening daily but nothing changed. Martin would later learn that the 24 tablets he was subjected to on a daily basis for one month did him more harm than good.
The doctors at Thika Level Five Hospital, unable to treat him and help him regain his eyesight as they had promised and after a series of misdiagnosis for 31 days, decided to refer him to Sabatia Eye Hospital in Vihiga County.
“At Sabatia, they told me they could not see any issue with my eyesight though at this time I had very little light perception which kept on diminishing,” he says.
He remained at the hospital for a long time until the doctors gave up and told him that his predicament “was now in the hands of God.”

Martin Imbalambala narrates how he lost his sight and was later diagnosed with glaucoma.
He was again referred to Lions SightFirst Eye Hospital in Loresho, Nairobi, where doctors established that he was battling glaucoma.
According to the Ministry of Health (MoH), glaucoma is a group of diseases that gradually affects the optic nerve. It is the second leading cause of vision loss globally and it continues to pose a challenge to eye health professionals in the country.
In the national guidelines for management of glaucoma, Dr Patrick Amoth, the acting director general for health at MoH, highlights that in Kenya it is estimated that 4.3 per cent of persons aged above 50 years have glaucoma after a population-based study was done in Nakuru.
“The blindness caused by glaucoma is irreversible. We know that if diagnosed early and with quality care, blindness due to glaucoma can be prevented,” he says. It disproportionately affects the black race. Africa has a high prevalence of glaucoma with the commonest type being primary open angle glaucoma (POAG).
The risk factors for POAG include being of African heritage, older age, high intraocular pressure (IOP), family history of glaucoma, type 2 diabetes mellitus, high myopia and thin central corneal thickness. Every person over 35 years of age is at risk of glaucoma.
Glaucoma is classified into three categories namely primary glaucoma, which includes primary open angle glaucoma, normal-tension glaucoma, low-tension glaucoma, ocular hypertension, primary angle closure glaucoma (acute, subacute, chronic), plateau iris syndrome and mixed glaucoma.
Secondary glaucoma includes secondary open angle and closed angle glaucoma while the third category, which is childhood glaucoma includes primary congenital glaucoma (PCG),glaucoma associated with systemic conditions and secondary paediatric glaucoma due to uveitis, ocular trauma, post infantile cataract surgery, retinoblastoma or retinopathy of prematurity.
“At first there are no symptoms. Vision stays normal and there is no pain. However, as the disease progresses, you may slowly lose side vision. Objects in front may still be seen clearly, but objects to the side may be missed,” the Health ministry explains while pointing out that glaucoma can develop in one or both eyes.
“If untreated, you will slowly lose your peripheral (side) vision. You will seem to be looking through a tunnel.”
When the Healthy Nation team visited Lions FirstSight Eye Hospital where Martin was diagnosed and is regularly treated, Dr Lily Nyamai, an ophthalmologist at the hospital who specialises in glaucoma, explained that the eye is a very intricate and interesting structure.

Dr Lily Nyamai, an ophthalmologist/glaucoma specialist at Lions SightFirst Eye Hospital, during the interview.
“The cornea and the lens are refractive surfaces in that they allow light to go into the eye through the pupil, which helps focus light onto a receptor which we call the retina,” she explained.
The retina, she added, has some special cells called retinal ganglion cells (RGC) that bear the sole responsibility of propagating visual stimuli to the brain.
These cells have fibrous nerves and are scattered throughout the retina at the back of the eye to form an important nerve called the optic nerve, which transmits messages to the brain. “This means that we use our eyes to perceive but the brain is what actually sees, because these fibres take these messages to the back of the brain,” Dr Lily added.
“Glaucoma is group of diseases, a degenerative process of the nerve of the eye. For most cases you don’t notice anything, which is why we call this disease a ‘thief of sight’.”
She highlighted that when a patient notices the symptoms, it is usually an advanced stage in most cases like what happened to Martin.
“Any degenerative condition that affects the nerve and is associated with peripheral loss of vision is defined as glaucoma. Sometimes patients may have very good vision in that they might see far but have a problem with noticing things on the sides and are unable to cross a road to a point that they have to turn their entire head to see.”
Dr Lily added that many patients who have glaucoma have high intraocular pressure (above 21 mmHg) in the eye though there is a group of patients who may have normal pressure but have glaucoma.
This makes pressure in the eye, the biggest risk factor.
She expounded: “The eye is like a ball and has to be kept turgid at a certain pressure. There are structures in the eye that produce a fluid that keeps the eye turgid and then there are also structures that drain it. Usually if there is a problem like over-production or drainage, this can raise the eye pressure. Modifying eye pressure is the only thing we can do at the moment in terms of treatment.”
This is done by administering eye drops known as intraocular, which are pressure lowering drugs apart from using special laser that are applied in the eye to help reduce intraocular pressure.
“We do have lasers that help open up the drainage in the eye around the coloured part known as the iris.
“In some people there is a drainage in the part where the cornea and iris meet. The coloured part of the eye sometimes blocks that drainage, many times it does reduce the eye pressure because when the drainage is blocked the pressure goes up,” Dr Lily explained, adding that they reduce the pressure in other cases by performing surgery depending on how advanced the disease is.
“We do a thorough eye examination and grade whether you are have mild, moderate or advanced glaucoma.”
According to Dr Lily, for patients who get glaucoma as a result of blocked drainage in the eye due to pressure, it can be more dramatic towards dusk when the coloured part of the eye falls back towards the drainage, which explains the painful headaches Martin suffered in 2018.
“They can experience nausea and when they look at light, they see rainbow hallows and distorted ashy images at first. They also want to stay in dark places — a type of glaucoma known as angle closure.
“Patients dealing with this kind of glaucoma have red-blood shot eyes, problems with light and a lot of headache and vomiting, it actually has symptoms.”
The glaucoma expert further highlighted that the condition is associated more with men than women.
Dr Lily also disclosed to Healthy Nation that they are seeing increased cases of young people in their thirties developing glaucoma.
She explained that genetics is another major risk factor, which is why they ask everyone to prioritise being screened.
“We should discuss this thing in our families and find out if things like glaucoma run, we can’t place why glaucoma has a heavy burden in people of African origin but epidemiological studies have shown that we tend to get a higher burden of glaucoma and we can get it earlier compared to other people.”
“For the main diseases that cause blindness — glaucoma and cataracts — age is another major factor.
“Diabetes, hypertension, arthritis and other diseases that have to do with lifestyle also are a risk factor as they lead to pressure in the eye,” she said while advocating for good diet and regular exercise.
“I usually say your plate should be half vegetables, the other quarter should be proteins while carbohydrates take the remaining quarter in moderate amounts,” Dr Lily said.
A cataract is a clouding of the lens of the eye.
This means that as a cataract develops, your eyesight may become cloudy, blurry or unclear.
For treatment, Dr Lily noted that they start with eye drops, laser treatment then surgery.
“Depending on the brand, generic eye drops go from Sh900 to Sh6,000. For the original ones, we have had a deal with drug makers to reduce prices and now the cheapest is going for Sh1,000,” she said.
For the laser treatment, the procedure costs Sh10,000 per session per eye. The procedure can be repeated after three to six months while for surgeries it depends on the type of operation that is needed though a package can be tailor-made for a patient if they are dealing with both glaucoma and cataract.
“Surgeries depend on whether you are doing it with your own eye tissue or a shunt (involves placing a flexible plastic tube with an attached silicone drainage pouch in the eye to help drain fluid known as aqueous humour).
“If it’s a shunt, it’s about Sh250,000 and if it’s a surgery with your own tissue, you will part with Sh50,000,” Dr Lily told Healthy Nation.
The ophthalmologist insisted on regular screening to have any signs of glaucoma detected early.
“Instead of losing vision much earlier in life, I have seen patients who embark on treatment early with their eyesight intact until their demise, thanks to treatment and medication,” Dr Lily said.
For Martin, he has accepted his new normal and adapted after graduating from the Kenya Institute for the Blind.