Malaria deaths, cases reduce with vaccine and drug combination
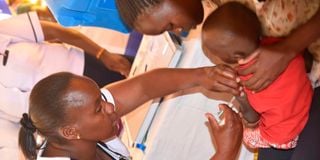
A nurse administers malaria vaccine to a child in Vihiga County on March 7, 2023.
What you need to know:
- The findings confirm the potential of seasonal vaccination to provide a high level of protection in young children in the first five years of life, a period when this protection is needed.
- Nearly half of childhood deaths from malaria are in children living in areas of highly seasonal transmission.
Final results of a five-year landmark study have confirmed massive benefits of combining malaria vaccine with antimalarial drugs in settings of highly seasonal malaria transmission.
According to the study published in the Lancet Infectious Diseases journal, giving young children the world’s first malaria vaccine RTS,S/AS01E (RTS,S) alongside antimalarial drugs has led to a significant reduction in life-threatening malaria cases and deaths.
The findings show that the vaccine-drug combination reduced clinical malaria episodes, including cases of severe malaria and deaths in young children by nearly two-thirds compared with either RTS,S vaccination or seasonal malaria chemoprevention (SMC) alone.
These findings confirm the potential of seasonal vaccination to provide a high level of protection in young children in the first five years of life, a period when this protection is needed.
The Phase three study coordinated by the London School of Hygiene and Tropical Medicine with partners Institut des Sciences et Techniques and Institut de Recherche en Sciences de la Santé, Burkina Faso; the Malaria Research and Training Center, University of Sciences, Techniques and Technologies of Bamako, Mali; and PATH, Seattle, Washington,, followed more than 5,000 children for five years.
The findings are consistent with those from the first three years, which were published in 2021. Those findings contributed to the World Health Organization’s (WHO) decision that year to recommend the RTS,S vaccine for use in settings of moderate-to-high malaria transmission, including its use in areas with highly seasonal malaria or in areas of perennial malaria transmission with seasonal peaks.
According to Prof Brian Greenwood, a member of the research team, during the study, children who received the RTS,S-drug combination and also used bednets likely had greater than 90 per cent protection against malaria episodes.
“This points to the importance of ensuring access to multiple malaria prevention tools for reducing the tremendous burden of the disease and deaths in these highly seasonal settings,” he added.
Prof Jean-Bosco Ouedraogo of Institut des Sciences et Techniques, also a member of the research team, said the challenge now is to determine how best to deliver the vaccine-drug combination and to follow these highly protected children as they grow older.
In light of what is already known about the potential for malaria “rebound” following the withdrawal of malaria prevention, children in the study who received SMC and/or the vaccine are being followed for a further two years.
This additional follow-up will help to determine how long protection lasts and whether the high level of protection against malaria provided by the combination of SMC and seasonal RTS,S impaired the acquisition of naturally acquired immunity among children in the study.
Currently, SMC is not given to children above the age of five years in most countries where it is deployed.
The newly published results come from a two-year extension of the Phase the study that began in Burkina Faso and Mali in 2017. The extension began in April 2020, when 5,048 (94 per cent) of the 5,433 children who completed the initial three-year follow-up were re-enrolled.
Over the full five years, protective efficacy of the RTS,S-SMC combination was very similar to that seen in the first three years, with protective efficacy of the combination versus SMC alone being 57.7 per cent and versus RTS,S alone, 59 7 per cent. The comparable figures for the first three years of the study were 62.8 7 per cent and 59.6 7 per cent, respectively. (The protective efficacy of each intervention alone could not be assessed because all children participating in the study received one or both interventions; there was not a group of children who received neither intervention.)
Compared with SMC alone, the RTS,S-SMC combination reduced by two-thirds hospital admissions for WHO-defined severe malaria (66.8 7 per cent), malarial anemia (65.9 7 per cent), blood transfusions (68.1 7 per cent), and malaria deaths (66.8 7 per cent).
“Our study showed that administering the RTS,S vaccine seasonally every year reduces the burden of malaria drastically in children under the age of five who are the most affected by this disease. Rapid implementation of this new additional tool is needed to reduce the huge burden of malaria on children in our countries,” said Prof Alassane Dicko, the Malaria Research and Training Center managing director and a member of the research team.
SMC, which involves giving antimalarial drugs sulfadoxine-pyrimethamine and amodiaquine to young children four or five times during the rainy season when malaria transmission peaks, is highly effective in preventing malaria and was recommended by WHO in 2012 for use in areas with highly seasonal transmission.
Continued testing of a subset of children in the study found that the drugs currently used for SMC remain effective in the study areas. However, the study authors concluded that seasonal vaccination with RTS,S could be a potential solution if resistance to the drugs increases and no alternatives are available.
“Nearly half of childhood deaths from malaria are in children living in areas of highly seasonal transmission. These data show the remarkable reduction in malaria that can be achieved by strategically delivering the vaccine with other effective interventions—and the potential for saving many young lives,” said Mary Hamel, senior technical officer at the WHO Product Development Research Unit and team lead for malaria vaccines.





