Why law requires seizing suspected rabies animals
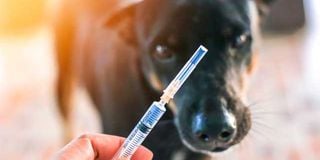
An animal health service provider prepares to treat rabies in a dog. Symptoms of the deadly disease include red eyes, frothing, dullness and hind legs weakness.
May 4, 2024 shall remain etched in my memory as one of the days I handled a case with possible devastating consequences, that fortunately never materialised.
I was busy doing a report when Emily, our admin, alerted me of boys with a sick dog in the waiting room.
She asked me to quickly attend to the animal as the children said the dog had bouts of fainting. In her opinion, the animal was very ill. She said the doctor on duty was busy with another patient while Dr Mwikali had already left for a house visit.
I trust Emily’s judgment and case scheduling because her many years of experience and operational training have positioned her to organise patients for the doctors available at any time at the clinic.
Newly-qualified doctors and students, encountering her in action for the first time, ask how she manages the work without formal animal health training.
I explain that professionals need to understand and appreciate that operational management is common in all fields of practice and is better carried out by people who are not trained in the particular discipline as long as they are initially trained in administration and well-trained in operations of the specific professional service they are employed in.
I found seven boys in the waiting room. One was holding a dog on a leash. The animal was coiled up under a seat and looked oblivious of its environment.
The boys appeared under 14 years. One stood out as the obvious leader of the troop.
He smiled, stood up and extended his hand to greet me.
I clenched my fist and gave him a “corona” greeting. The dog’s posture and red eyes immediately raised my rabies antennae. Greeting the boy with an open hand could expose me to the rabies virus.
Saliva foam
Emily gave me a disapproving look and shrugged out of sight of the children. She later explained to me she thought my action was customer unfriendly. She had quickly changed her mind when she heard me tell the boys to thoroughly wash and disinfect their hands immediately.
The dog was a rabies suspect and the boys who had handled it were probably exposed to the virus.
One of the boys said he had wiped off saliva foam from the dog’s mouth with his bare hands to keep the animal clean.
Francis, the band leader, demanded to know why I thought the dog was rabid, yet it appeared very calm and had not attacked them.
They had walked with the animal for about two kilometres. The only thing they observed was weakness in the hind quarters and the animal would tire easily and collapse.
That was the only reason they had brought it to the clinic.
Readers of this column may recall I have narrated cases of rabies in cattle and dogs.
However, each has a different perspective that helps understand the various aspects of the deadly disease.
In this case, the history of hind leg weakness, frothing at the mouth, dullness and inability to swallow two doughnuts the boys had given the dog were rabies infection red flags.
The red eyes I observed, even without touching the dog, further enhanced my suspicion.
After getting the history and making observations, I secured the dog with a catcher, fitted the mouth with a muzzle and continued examining it closely.
The eyes were very red, there was dried saliva on the lips and two bite wounds on the face. The lymph nodes were swollen and the dog had lots of ticks. The animal failed the water test.
Dogs with rabies show hydrophobia or fear of water. They turn away their heads when water is presented to them to drink.
This reaction is caused by a painful throat due to paralysis of swallowing muscles caused by rabies infection. Even water swirling causes the dog to turn its head away from the direction of the sound.
Rabies infection
I took some blood for in-house lab analysis. The results showed dehydration and some blood parasites spread by ticks. It is the parasites that had caused the swelling of the lymph nodes.
I treated the dog for the dehydration and blood parasites. I then explained to the children that their innocence had made them vulnerable to rabies infection.
They had seen a dog mistreated by other children and made to fight another dog. That is how the animal got the bite wounds on the face.
The boys had decided to bring the dog for treatment at the clinic, oblivious of the danger they were in.
Fortunately, the animal had the dumb form of rabies where the patient is deeply depressed and prefers to coil and rest.
I told the boys that the animal would remain at the clinic until we confirmed if it had rabies or not.
They protested they only had Sh100 and could not afford the treatment and admission cost.
I explained the matter was no longer about money but their safety, that of their community and the other animals in the village, including cows, goats and pigs.
The law requires us to impound all rabies-suspected animals presented at the clinic, confirm the disease and report to the veterinary and health authorities.
We agreed with the children that they would bring their parents to the clinic because they could not legally make decisions.
On May 7, the National Veterinary Research Laboratories in Kabete confirmed the dog indeed had rabies.
The rabies confirmation report started a new cascade of events that are ongoing. I shall narrate it in future.





