Africa can flatten Covid-19 curve only if it invests in own health ecosystems
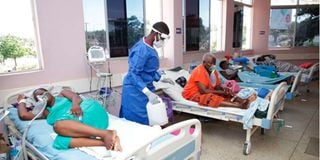
A nurse attends to Covid-19 patients recuperating at Jaramogi Oginga Odinga Teaching and Referral Hospital in Kisumu County on June 10, 2021.
Covid-19 has shown what African governments, philanthropists, pharma and science institutions can achieve when they work together. But it is also devastating our fragile health workforces, detracting investment in health infrastructure and making vital healthcare services grind to a halt.
These include the suspension of childhood vaccination programmes, HIV testing and anti-retroviral therapy initiations, mental health services and sexual and reproductive health services. It is also setting back control of malaria and neglected tropical diseases through mass drug administration.
As countries revise their budgets to minimise the economic impact of Covid-19, the fallout could be catastrophic for some health programmes in Africa reliant on overseas aid. To minimise the impact, African governments must reallocate funding to health to close the gap between the budget and the actual expenditure. They also need to retain and draw on local personnel, expertise and innovation to reduce operational costs.
Clinical trials
Medicines regulatory authorities must develop permissive frameworks that support, not stifle, local innovation. Philanthropists and pharma must invest in local infrastructure, clinical trials and mass production. Researchers and innovators must undertake international standard research and clinical trials on local medicines and interventions.
There are already calls for Africa to reduce its 2030 UN Sustainable Development Goals targets and focus instead on the African Union’s longer-term Agenda 2063 goals. This will only delay the problem. With a rapidly growing and young population, we bear the largest burden of infectious diseases and a growing burden of metabolic diseases.
We must invest in local personnel, practices, systems and products. Such an ecosystem will enable African health systems to continue functioning during a health emergency and also recover from one quickly.
Every year, Africa trains tens of thousands of medical personnel, scientists and innovators, who then leave to work abroad. The brain drain costs Africa an estimated $2 billion (Sh200 billion) yearly in the health sector.
Local investment is key. It provides autonomy, stability and sustainability to improve health provision and health systems. The UK’s recent decision to cut its aid budget from 0.7 to 0.5 per cent of GDP is just the latest example, which has translated into immediate cuts of up to 70 per cent in global health research funding and 90 per cent in other programmes in Africa’s Sahel region.
Pharmaceutical innovation
Pharmaceutical innovation and production is another area where Africa is terribly reliant on external suppliers. More than 80 per cent of the medicines sold in Africa are imported. Prioritising and drawing on unique African knowledge and experience, we can deliver solutions in our own settings.
Rwanda has drawn lessons from Ebola to respond to the pandemic using drones to disseminate information, robots for Covid-19 screening and inpatient care, and social media for official health communications. Ethiopia uses the African Ubuntu philosophy to shield vulnerable community members from Covid-19. South Africa is engaging its deep network of community health workers for Covid-19 testing and education.
With adequate investment, therefore, African interventions can be highly successful.
But Covid-19 also highlights Africa’s failure. A Covid-19 vaccine candidate discovered by Nigerian scientists did not progress due to lack of funding. The only current large-scale drug clinical trial for Covid-19 therapeutics in Africa (Anticov) is externally funded.
Like elsewhere, Africa’s economy has been battered by Covid-19, shrinking by 5.3 per cent in the year to December 2020. But focusing on economic recovery alone is short-sighted. Good health underpins economic growth, providing many times its face value through lasting improvements to productivity and economic growth stimulated by health innovation, pharma and research.
Without these elements, African health systems will continue to haemorrhage lives.
[email protected] @PIG_Edinburgh





