Dr Bosire: The skeletons in the medical field
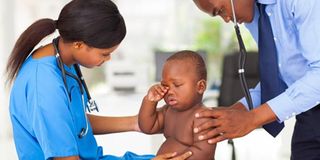
Stress among doctors is amplified when patient care is not achieved.
What you need to know:
- For years, physicians have been viewed as super-beings, rightly because it is in their hands that pain is alleviated, lives are saved and suffering due to disease is eradicated.
- But one reality that as a society we have failed to recognise is the political, social and economic obstacles that have compromised service to humanity and that ultimately affected the mental wellbeing of physicians.
I started my morning today with a grief debriefing session with my therapist Joan Kirera. Her first question was: “Why has the death by suicide of your colleague triggered you and many doctors?”
She was referring to Dr LN who died suddenly and unexpectedly on June 12th, in her car at Kenyatta National Hospital. Dr LN was on management for mental illness.
I paused for a moment because I did not know if I should speak of our collective undergraduate experience or the experiences of those in post-graduate- because both these experiences are in continuous exposure to trauma and burnout. For years, physicians have been viewed as super-beings, rightly because it is in their hands that pain is alleviated, lives are saved and suffering due to disease is eradicated. But one reality that as a society we have failed to recognise is the political, social and economic obstacles that have compromised service to humanity and that ultimately affected the mental well-being of physicians.
What burnout does
Burnout drains energies away and ultimately influences our happiness, how we relate to others, career satisfaction and patient care. Now imagine in a year of a pandemic where your place of work is akin to a battlefield; when you leave your house in the morning, you are not sure if you will survive the day. You are working long hours, under difficult conditions, you are not well protected and could contract Covid-19 every time you are exposed to patients, you are also grieving the loss of patients and are heartbroken by a family that has lost a loved one too; worst still, you are not sure if you could be the next statistic in death-Kenya has lost more than 35 doctors since the Coronavirus-19 pandemic raged in March 2020.
Relationships are affected
Burnout also affects how physicians build and maintain personal relationships. Physicians often spend 60-80 hours per week away from their loved ones while working or studying. This negatively affects their relationships outside work. Chronic burnout empties one’s energy cup to levels personal relationships becomes work, yet, this was initially something which was once enjoyed. In burnout one is constantly moody, withdrawn, apathetic and very unpleasant to be around. No relationship can thrive in such an environment.
Stress levels within medical training is worsened by abusive colleagues, mostly those who are senior and therefore yield power. This power is often so grand that it can determine one’s career fate. Often, this power is expressed in the form of verbal abuse, either as abusive language, ignorance, condescending behaviour and intimidation. It makes the workplace very toxic. As a coping mechanism, most of those who are abused either numb it, or gradually start having issues with confidence, esteem or imposter syndrome.
Stress is also amplified when optimum patient care is not achieved. During the Kenyan physician’s strike, one common phrase that was often heard in the media was, ‘’We are tired of supervising and diagnosing death’’, a phrase that exposed the weak system where doctors trained to save lives are so helpless that they can only resort to recording death. The Covid-19 crisis has worsened this. We have lost patients because we run out of essential medicines, because there was no ICU bed or because we ran out of oxygen. I have once broken down privately when a patient I was managing some years back was diagnosed with an incurable disease and whose prognosis was so bad that it would have taken a miracle for them to live beyond six months. This was a very jolly, young and full of life person, and who had grand plans about their life- I was heartbroken for a long time. So, never assume that the outcomes of our patients never affect us, we are just trained not to express it before you.
Substance abuse
We cannot fail to mention the issues of substance abuse among physicians. While there are few studies done to quantify the burden of substance use among healthcare workers in Kenya, this study indicated that healthcare workers are more likely to abuse prescription medicine mainly to relieve stress, physical or emotional pain, and this rate varying according to specialisation; with the rates of substance abuse being higher in anesthesiologists, emergency medical doctors, psychiatrists and those in the surgical careers. Substance abuse in multiple studies is correlated with a higher rate of death by suicide, with a higher occurrence in males compared to their female counterparts.
Like other doctors, I often find myself overwhelmed by the pressures of life; sometimes the pressure is so much that I need help to cope, hence my normalisation of psychotherapy. We need to normalise therapy and destigmatise the shame that is associated with seeking help from physicians. Teaching institutions need to review their curriculum so that time can be availed for those who need to seek the help of a mental health nature, as well as ensure that residency or undergraduate education is not a precursor to severing personal relationships. We need to advocate for the creation of counselling programs that are confidential and which can be accessed by medical students in training without victimization or exposure. We must also create an environment where physicians battling mental illness can speak about their illness without it being weaponised to end their career.
***
Dr Stellah Bosire is a Medical Doctor, Human Rights Activist and student of Law.