I got the first malaria vaccine in Kenya and this is how I've been feeling
What you need to know:
- Despite using treated mosquito nets, Ellian would still get infected.
- He was diagnosed with malaria when he was five months old.
- He was admitted for four days with serious fever, vomiting and diarrhoea.
- Using the world’s first vaccine, Ellian became the first child in Kenya to receive the jab.
On September 13, 2019, Ms Noreen Kiminy prepared her son and left for Got Agulu Sub-County Hospital in Ndhiwa, Homa Bay County, for routine immunisation.
Ellian, who was turning six months, was due for his tetanus and flu vaccines.
To Ms Kiminy’s surprise the hospital had on the very day launched the routine vaccination of infants against malaria.
Ms Kiminy recalls being hesitant about allowing her son to get vaccinated, given that Ellian was going to be the first child to receive the jab in Kenya. She was also unsure about the vaccine’s safety. “I remember asking myself ‘what if the vaccine is not safe?’,” Ms Kiminy tells HealthyNation.
Despite assurance from health experts and even the then Health Cabinet Secretary Sicily Kariuki, who launched the immunisation programme, she was still not convinced the vaccine was good for her son.
Leading killer
“I knew the vaccine would protect him from malaria, but I needed a family member’s assurance so that in case of any eventuality, I would not take all the blame,” says the secondary school teacher.
She consulted her husband, a clinical officer, and her mother. They advised her to get Ellian vaccinated.
“They did not even think twice. They assured me the boy was going to be okay and that it was to his advantage because he used to have severe fever frequently, which had once led to his hospitalisation,” she says.

Despite using treated mosquito nets, Ellian would still get infected and was diagnosed with malaria when he was five months old.
He was admitted for four days with serious fever, vomiting and diarrhoea.
Using the world’s first vaccine to combat a disease that kills 800 children globally daily and a leading killer of children under five in Kenya, Ellian became the first child in Kenya to receive the jab.
Ellian has since completed his four jabs. “Ever since he got vaccinated, he has not suffered any episode of malaria. But, we are still sleeping under a treated mosquito net,” she tells HealthyNation at Got Agulu Sub-County Hospital.
Got Agulu Sub-County Hospital was the first facility to administer the malaria vaccine in the country.
At the hospital, women are carrying their babies on their laps waiting for their children’s turn to receive the malaria vaccine.
One by one they go in. A nurse prepares the vaccine by tapping on the syringe to dislodge bubbles, she explains the procedure to each woman, and writes down the serial number of the vaccine in her record book and in the clinic vaccination booklets.
“We are going to administer the vaccine in the left arm. Kindly remove all the clothes and prepare the baby,” the nurse tells Mama Sharon.
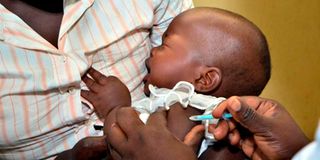
Seven-month-old Queensly Harriet receives her second dose of the malaria vaccine at Got Agulu Sub-County Hospital in Homa Bay County on April 16.
The procedure is repeated on other babies, some of whom were getting their final dose of the vaccine.
Since inception, about 29,944 children have received their first dose of the malaria vaccine in Homa Bay County. About 17,321 have received their second dose while 12,518 children have one dose left, according to the county immunisation coordinator, Rosemary Ongete.
About 560 children in Homa Bay have finished the fourth dose, a landmark in the battle against a disease that still remains one of the top 10 causes of death in the country despite rapid interventions.
Coupled with other interventions, the vaccine has since seen a reduction in the malaria prevalence for under five children.
Malaria prevalence in lake regions has dropped from 27 per cent in 2015 to 19 per cent in 2020, according to the Malaria Indicator Survey 2020.
Data from Ndhiwa shows malaria has reduced from 62 per cent in 2018 to 39 per cent last year.
In Homa Bay County, only three sub-counties including Ndhiwa, Homa Bay town and Kabondo are in the phased approach as they scale it to other sub-counties.
Severe cases
The vaccine, integrated with other interventions, has reduced the number of severe cases of malaria and blood transfusions in most hospitals in the county.

Mothers wait to get their children vaccinated at the Yala Sub-County Hospital in Siaya County on April 19.
According to the World Health Organization, the vaccine has the potential to save tens of thousands of lives. However, it is limited to the poorest parts of the world since it is not clear if it will be feasible to use.
In Kenya, the vaccine is given to babies in four doses: the first one at six months the second dose at seven months, the third one is given at nine months while the last dose is given at 24 months.
In the clinical trials, the vaccine decreased malaria cases by 39 per cent and severe cases by 29 per cent. Though it can only be effective if the children receive all the four doses, this can be challenging for many families who live in the rural areas and are far from health facilities.
The researchers from the trials found out in children who got the four doses of the vaccine, it prevented about 40 per cent of all malaria cases.
With the piloting of the vaccine being carried out in three countries, Ghana, Malawi and Kenya, WHO will then assess the safety and effectiveness of the vaccination.
The three countries, according to WHO were chosen because despite running large programmes and interventions to tackle malaria, including the use of bed nets, they still have a high numbers of cases.

Loice Otieno, who is eight weeks pregnant, receives a treated mosquito net from a nurse at the Yala Sub-County Hospital in Siaya County on April 19.
Kenya has made tremendous progress in the fight against malaria including scale-up of insecticide-treated mosquito nets (ITNs), indoor residual spraying with insecticides and appropriate diagnosis and treatment using artemisinin-based combination therapies but the disease remains stubborn.
Testing rate
Admission for malaria in children under five has also reduced from 178 to 62 cases. Mr Robert Bonyo, Homa Bay County Malaria Control Coordinator, says the uptake of the vaccine among children below two years in the county stands at 70 per cent.
“This is one of the interventions that is helping us to control malaria in the county. The demand is high in other sub-counties that are not implementing it,” he says.
With the integrated malaria interventions, there is a drop in cases, he adds. The number of confirmed cases in Homa Bay County has been declining over the years from over 500,000 in 2016 to less than 150,000 in 2020.
Malaria test positivity rate has also been declining from 38 per cent in 2016 to 18 per cent last year due to an increase in testing rate and integrated prevention and control measures.

Olga Adhiambo (left) removes household items from her house before Indoor Residual Spraying is conducted at her homestead in Disii Village, Homa Bay County on April 16.
Nationally, out-patient attendance has since reduced from 30 to 19 per cent, and in-patient admissions have dropped from 20 to 15 per cent. The number of confirmed malaria cases decreased from 113 per 1,000 of the population per year in 2016 to 86 per 1,000 per year in 2020.
Experts say more efforts are geared towards ensuring reduction of malaria cases to attain the goal of reducing malaria incidence and deaths by 75 per cent of the 2016 level by 2023.
In Kenya, the pilot was being conducted in eight counties: Homa Bay, Migori, Kisumu, Siaya, Busia, Bungoma, Vihiga and Kakamega. Only Homa Bay and Migori have since introduced indoor spraying with insecticides.
According to Zeddy Bore, the US President’s Malaria Initiative VectorLink Project Operations Manager, they cover 14 sub-counties in Homa Bay and Migori applying the long-lasting residual insecticides inside the walls of houses.
Last year, they covered 94 per cent of structures in Migori and 87 per cent in Homa Bay. In total, 1.7 million people were covered.
“For the past four years since 2017, we have been using phosphate. However, this year, it was changed to fludora fusion which is a combination of pyrethroids and clothianidin and we have since adopted a policy to rotate the different insecticides,” says Ms Bore.
Pilot period
The insecticides can last in the walls for nine months, covering both the long and short rain periods.
As the world celebrated the World Malaria Day, with the theme “Zero Malaria - Draw the Line Against Malaria”, African children are at the highest risk of malaria deaths.
The three pilot countries are yet to release data on malaria prevalence after the introduction of the vaccine, but the statistical analysis is ongoing. The data will be available once the pilot period is over.

A technician with the US President’s Malaria Initiative conducts indoor residual spraying in a homestead in Disii village, Homa Bay County, on April 16.
It is expected that an updated WHO policy recommendation would be achieved later this year to guide recommendations and expanded use of the vaccine in Kenya.
According to data from the three countries, more than 1.7 million doses of the malaria vaccine will have been administered by Ghana, Kenya and Malawi, and more than 650,000 young children will have received a first dose of the vaccine.
Ghana is leading with the number of doses administered. More than 680,000 doses of the vaccine will have been administered, with nearly 240,000 children having received the first dose by the end of April. Then Malawi where more than 620,000 doses of the vaccine will have been administered, with nearly 230,000 children having received the first dose by the end of April.
In Kenya, more than 450,000 doses of the vaccine will have been administered, with 190,000 children having received their first dose by the end of April.
The vaccine, in all the three countries, was added to the national immunisation schedule. Like in Kenya, children in Ghana receive the vaccine from six months old, with the final dose given at around 24 months.Malawi administers the jab to children from five months old, with the final dose given at around 22 months of age.

Homa Bay County Coordinator Robert Bonyo speaks on the region's actions and preparedness on the detection and prevention of malaria on April 16.
Currently, there is no malaria vaccine that has been approved for use in the world. However, the RTS, S vaccine, its brand name Mosquirix, is the most advanced in the development process. It was first created in 1987.
The vaccine took long to be developed because the malaria parasite has a complex life cycle.
Mr Bonyo emphasises that vaccines alone will not eliminate malaria.


