Cancer care: How climate change is impacting diagnosis and treatment
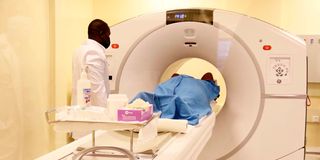
A patient undergoes cancer screening at the Integrated Molecular Imaging Center located at the Kenyatta University Teaching Referral and Research Hospital on January 10, 2022.
What you need to know:
- In Africa, different cancers killed 700,000 people in 2020 alone, according to data from the Institute of Health Metrics and Evaluation.
- In Kenya, cancer was the third deadliest killer in 2019, taking 23,000 lives.
For three decades now, cancer has been one of the most dreaded diseases in the world, killing 10 million people every year. In Africa, different cancers killed 700,000 people in 2020 alone, according to data from the Institute of Health Metrics and Evaluation (IHME).
In Kenya, cancer was the third deadliest killer in 2019, taking 23,000 lives. IHME data on the global burden of disease shows that cancer incidence in Kenya and Africa has been on an upward trend in recent years. But with advancements in medical technology, it has become possible to identify and control cancer risk factors, improve early detection and develop effective cancer therapies.
But there is a new threat. Experts say climate change has complicated cancer care in the world by increasing exposure to cancer risk factors and access to care for cancer patients.
Curiously, though, the discourse on climate change centred on its impact to the environment, food security and other facets of human life for many years. It was not until recently that experts started to link the phenomenon to devastation of human health.
According to an article titled ‘‘Climate Change and Cancer’’ published in CA: A Cancer Journal for Clinicians, climate change is increasing the risk of cancer through increased environmental and even dietary exposure to carcinogens.
Carcinogens are elements that cause cancer. Aflatoxin, for instance, is a potent carcinogen that is produced by fungi. It is known to contaminate food crops such as maize and wheat, considered Kenya’s staple foods.
This situation is worsening by the year, especially in Africa, disrupting care, impacting survival of patients and driving higher mortality rates.
Stakeholders in health drawn from Africa recently launched a programme dubbed Accelerating Cancer Treatment (ACT) that will look at the state of cancer care in Africa, addressing the gaps and challenges and exploring areas of collaboration between players for better interventions. The event that was hosted by pharmaceutical multinational AstraZeneca was held on the sidelines of the just concluded COP27 in Sharm-el-Sheikh, Egypt.
Dr Githinji Gitahi, the global CEO of Amref Health Africa, says 75 per cent of all cancer cases are diagnosed at Stage Four, complicating treatment and, in most cases, losing the patient soon after.
"We need to bring forward prevention, screening, early diagnosis and early treatment for patients to have a chance at survival,’’ says Dr Githinji. He notes that early screening for cancer is an economic intervention for countries considering the high cost of care for patients.
"If you are diagnosed late, there is the cost of surgery, radiotherapy and chemotherapy. This could also result in loss of life. If you diagnose cervical cancer at Stage One, for instance, the cost of treatment is lower and the possibility of survival high,’’ he says.
Economically active
This, he adds, helps to make savings on future care for the patient while allowing the individual to continue being economically active.
Nigerian radiation oncologist, Dr Bello Abubakar Mohammed, says that while there is a higher incidence of cancer cases in developed countries, mortality is lower. He attributes this to developed infrastructure and capacity for treatment of cancer. ‘‘It is important to prevent cancers that are preventable through screening and vaccination. Preventable cancers account for 40 per cent of all our cancers.’’
According to Dr Bello, investment in treatment equipment is critical in the fight, an avenue where Africa is currently failing. ‘‘With a population of 1.3 billion, Africa would need about 5,800 radiotherapy equipment. There are less than 300 on the continent at the moment. About 22 countries in Africa do not have a single unit of the radiation machine.’’
In some African countries, cancer patients are handled by general practitioners. ‘‘We need to build the capacity of our doctors because cancer treatment is a specialised area.’’
Many developed countries lost their oncologists to Covid-19, according to Dr Bello. They are now coming for Africa’s oncologists in hundreds, further straining the continent’s capacity. ‘‘They are giving our doctors better incentives and taking them away because they consider doctor to patient ratio.’’
Those that remain on the continent, he says, suffer from acute fatigue syndrome, and end up not giving their best to patients. ‘‘A scenario of a cancer doctor attending to 100,000 patients is not acceptable anywhere.’’
Dr Mary Nyangasi who heads the National Cancer Control Programme at the Ministry of Health says public-private partnership is critical in boosting screening of cancer in Kenya and in Africa and for empowerment of patients.
"Our African people do not know much about cancer. When one is diagnosed with any cancer, they see it as a death sentence because of the stigma. We have collaborated with the civil society to develop educational material for cancer awareness among patients. We also provide tips on self-care to them,’’ says Dr Nyangasa. Meanwhile, access to and the quality of cancer care in Kenya is low, forcing hundreds of patients to seek treatment in Egypt and India.
"About 80 per cent of the treatment cost for the majority of non-communicable diseases such as cancer and hypertension is borne by the individual. We are not covering the financial protection of patients,’’ Dr Githinji says, and adds that governments in Africa must incorporate cancer care in their national health insurance schemes to lessen the burden on patients.
Cancer is painful, and management of pain, or palliative care, is critical. Dr Bello says patients can be palliated for as long as possible, just like in other terminal illnesses such as diabetes and hypertension.
Here, morphine comes in handy, he says. ‘‘Morphine production in Africa is so backward. Countries need to be able to produce their own to palliate their patients.’’ Kenya, Rwanda and Malawi are some of the African countries producing their morphine locally through initiatives between the government and non-profit organisations.





