Why devolving health docket was a bad idea
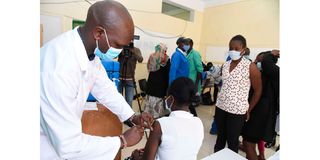
A nurse at a sub-county hospital administers a Covid-19 jab in 2021. Experience has taught us that healthcare cannot be run in 47 different ways and succeed.
Devolving healthcare, the process of transferring responsibility for the services from the national to county governments, has been a topic of debate for many years. While some proponents of devolution argue that it can increase efficiency and decision-making, there are many demerits associated with it.
Experience has taught us that healthcare cannot be run in 47 different ways and succeed.
First, it has led to an unequal distribution of resources and services. Counties do not have the funding or resources to provide adequate healthcare to all citizens, especially those in remote or economically disadvantaged areas. This has created disparities in access and outcomes, exacerbating existing social and economic inequalities.
Secondly, it has fragmented services. As the responsibility for healthcare shifted to multiple stakeholders, coordination and integration between services were lost. This resulted in less effective and efficient service delivery and an increased likelihood of medical errors and miscommunications.
Thirdly, it has caused a decline in the quality of care. Leaving healthcare to local governments, which do not have the necessary expertise or infrastructure to provide high-quality healthcare services, resulted in poorly trained health workers, outdated facilities and inadequate equipment or supplies, clearly compromising patient safety and health outcomes.
Fourth, it has led to a lack of accountability and oversight. Without centralised leadership and governance, it has become difficult to monitor and regulate healthcare providers, ensuring that they are delivering safe, effective and ethical care. This has led to situations where providers have engaged in fraudulent or unethical practices or provided substandard care without fear of repercussions.
Implications for public health
Lastly, it has had implications for public health. As counties manage their healthcare services independently, they may prioritise localised concerns over broader public health goals. This has resulted in a lack of investment in disease prevention and control strategies, which can have negative consequences for individuals and the wider community.
While some may argue that devolving healthcare brought services closer to the people, this pales in comparison to its near-catastrophic impact. In addition, this line of thinking does not scrutinise the quality of healthcare.
While it may have some potential benefits, the negative impact cannot be ignored. From inequalities in access to healthcare to fragmentation of services and a decline in quality of care, the drawbacks of devolution should be considered before implementing any changes in healthcare governance.
Any steps towards devolution should take into account the need for centralised leadership, oversight and accountability to ensure the provision of high-quality, equitable and effective healthcare services for all.
Dr Mwachi is the national chairman of Kenya Medical Practitioners Pharmacists Dentists Union (KMPDU). [email protected].



